Online Psoriasis Treatments & Prescriptions
* Includes Free Private Prescription & Consultation.
† Applies to UK only.

START YOUR TREATMENT TODAY
Available Treatments for Psoriasis
VIRTUAL HEALTHCARE
What to Expect From Your Online Video Consultation


How do I check if I’m eligible for a video consultation?
Video consultations are suitable for most patients who do not need a physical examination. They may not be appropriate if you require hands-on physical examination or need laboratory tests that cannot be done remotely. Video consultations are not a substitute for your regular doctor if you have a serious or life-threatening condition.
How do I complete my health profile?
Before booking, ensure your health profile is up to date. Your clinician will use this information to provide safe, personalised care. You may need to provide current medications and supplements, known allergies and adverse reactions, existing medical conditions, previous surgeries or hospitalisations, family medical history (where relevant), current symptoms or health concerns, height and weight (for BMI calculation), and blood pressure readings (where required).
How do I check my device is ready for a video consultation?
Make sure NowPatient has permission to access your camera and microphone, you have a stable internet or Wi-Fi connection, and you are using a compatible smartphone, tablet, or PC.
How do I select a service?
Log in to your NowPatient account and navigate to the relevant Service Card on your homepage. Follow the prompts for the service you need (e.g., NHS Pharmacy First, Weight Loss, Buying Treatments Online). Please remember, some services have eligibility requirements before you can book a consultation.
How do I choose a date for my appointment?
Select your preferred consultation date. You can add notes at this stage to help the clinician prepare for your session. Click Continue.
How do I choose a time for my appointment?
Select your preferred appointment time from the available slots and click Continue. Slots are available up to 7 days in advance.
How do I choose a clinician?
Browse available clinicians trained for your chosen service. You can filter by gender or spoken languages. Each clinician's full name, licence number, and specialist credentials are displayed. Select your preferred clinician and click Continue.
How do I review my booking?
Check the summary of your appointment and read the Pre-consultation Requirements for tips on how to prepare. Click Continue.
What safety information do I need to provide?
Enter your consultation address (where you will be during the call) and emergency contact details. You can also opt in to receive an SMS reminder 30 minutes before your appointment.
How do I confirm my booking?
Click Confirm Booking. You will receive an in-app confirmation pop-up, push and in-app notifications, and a confirmation email with details of what to expect.
How do I take my blood pressure via the app?
Some services require a recent blood pressure reading before your consultation. If prompted, open the blood pressure tool in the NowPatient app, read and agree to the disclaimer, enter your age, height, and gender, and follow the on-screen instructions. The tool uses your smartphone's front-facing camera — no cuff or wearable required. Classified as a Class I Medical Device (CE and UKCA certified). Available on iOS and Android only.
How do I join my video consultation?
At your scheduled time, open the NowPatient app and join your consultation.
How does identity verification work?
Your clinician will introduce themselves and verify your identity. Please have your ID ready.
What declarations do I need to confirm?
You will be reminded that you must complete the consultation for yourself, disclose all medical conditions, illnesses, and operations, disclose all prescription medications you are currently taking, and provide accurate and honest responses throughout. Withholding or providing false information can severely harm your health.
What happens during my clinical assessment?
Your clinician will carry out an assessment relevant to your chosen service. Depending on the service, this may lead to issuance of a prescription (added to your cart), guided counselling, discussion of test results, or general health advice.
What does it mean to consent to inform my doctor?
With your consent, your clinician may inform your regular doctor of the consultation outcome. NowPatient strongly recommends agreeing to this, as your GP is responsible for your overall care.
How will I receive my post-consultation summary?
You will receive a notification summarising the outcome of your appointment, any referrals made to your doctor, and any advice given by your clinician. If a referral letter was issued, you can view it in the Documents section of your account.
How do I complete my order if treatment was prescribed?
If your clinician prescribed a treatment, go to your Cart, complete any payment exemptions (such as NHS Exemption Declaration if applicable), select Checkout, choose your delivery address and method, confirm your billing address, review your order and submit payment. Your order will be sent to NowPatient’s licensed online pharmacy for processing and dispatch.
How do I complete the feedback survey?
You may receive a short survey about your experience. NowPatient encourages all patients to complete it — your feedback helps improve the service for everyone.
How do I cancel a video consultation, and what happens if I miss my appointment?
To cancel an appointment:
Go to the Consultations section of your account.
Select Upcoming Consultations.
Choose the appointment you wish to cancel.
Click Cancel and confirm.
Please cancel at least 24 hours in advance.
Missed appointments: After two missed appointments, your booking rights will be temporarily revoked. Contact the NowPatient support desk if you believe this was applied in error.
How do I contact NowPatient for help and support?
Contact Method | Details |
UK Phone | +44 20 388 51 500 |
US Phone | 1-866-967-1977 |
Hours (UK) | Monday–Friday, 9am–6pm GMT |
Hours (US) | Monday–Friday, 8am–5pm EST |
Support |
HOW IT WORKS
Common Questions About This Service


What Conditions Does the Get Treated Privately Service Treat?
NowPatient clinicians can assess and treat the following 30+ common conditions through the service
Hair loss
Weight loss
Insomnia
Menopause
Acne
Cystitis
Erectile dysfunction
Fungal nail infections
Genital herpes
Hair loss
Influenza
Irritable bowel syndrome (IBS)
Migraines
Psoriasis
Rosacea
Shingles
Thrush
Urinary retention
+ More
Who Is Eligible?
You can use the Get Treated Privately service if you:
Are aged 18 or over
Have a NowPatient registered account
How Much Does the Service Cost?
The consultation itself is completely free. If your clinician prescribes medication then you only pay for the cost of the medication, including any shipment costs. If your clinician does not prescribe a treatment, then there is no cost whatsoever.
The Get Treated Privately service follows a straightforward process:
Search for a treatment or condition. Log in to your NowPatient account and navigate to the Get Treated Privately Service Card on your account homepage. Use the Options Menu to search for a particular treatment or a condition that you would like get treated.
Complete your health profile. Before booking a consultation, make sure your health profile is up to date (see ‘Preparing for Your Consultation’ below).
Book a consultation. Choose a convenient date, time, and clinician. You can filter clinicians by gender and spoken languages. Booking slots are available up to 7 days in advance.
Attend your video consultation. Your clinician will verify your identity, review your health profile, assess your condition, and discuss treatment options.
Receive your treatment. If a prescription is issued, the medication is added to your Cart. Complete checkout and payment, and your order is dispatched from our licensed online pharmacy.
Preparing for Your Consultation
To ensure safe and personalised care, you must complete or update your health profile before booking. This helps your clinician identify potential drug interactions, allergies, and contraindications. Depending on the treatment or the condition being treated, Your clinician may require the following:
Current medications and supplements
Known allergies and adverse reactions
Existing medical conditions
Previous surgeries or hospitalisations
Family medical history (where relevant)
Current symptoms or health concerns
Blood pressure readings (see below)
Height and weight (to calculate your BMI)
Certain blood test results
Important: Before your consultation please ensure NowPatient has access to your device’s microphone and camera. Also please bring your ID - your clinician will verify your identity for safety. Finally, you can bring a carer, friend, or family member if they are in the same location as you. Let your clinician know at the start of the appointment. You may be asked about their relationship to you.
Providing Your Blood Pressure Reading
For certain medications or condition treatments, your clinician may need your most recent blood pressure reading. The NowPatient app uses an innovative, cuffless approach — your smartphone’s front-facing camera measures your blood pressure while held in front of your face. It is the world’s only blood pressure check without a cuff or wearable.
The blood pressure tool is classified as a Medical Device and conforms to EU CE and UKCA Class I Medical Device standards. CE Class IIa conformity is expected in 2025. You will need a recent iOS or Android smartphone with a front-facing camera (not available on desktop devices).
To take your reading:
Start the process. During booking, if a blood pressure reading is required, you will be prompted to take one via the NowPatient app.
Read and agree to the disclaimer.
Enter your personal details. You will need to provide your age, height, and gender.
Follow the on-screen steps. We recommend being in a well-lit room with a stable Wi-Fi connection. The screen will tell you when to stay still.
Attend your consultation. Your clinician will now have your most recent reading to make safe prescribing decisions.
What Happens During the Video Consultation?
At the start, your clinician will introduce themselves and confirm your identity. You will be reminded that:
You are completing this consultation for yourself and to the best of your knowledge
You must disclose any medical conditions, serious illnesses, or operations
You must disclose any prescription medications you are currently taking
You must provide accurate and honest responses since withholding or providing false information can severely harm your health and may result in life-threatening consequences
You confirm that your responses are truthful and accurate
Your clinician will then conduct the assessment relating to your chosen treatment or condition. At the end of the consultation, the clinician will decide whether treatment is safe and suitable for you.
If treatment is appropriate, the clinician will discuss the available options with you so that you can jointly agree on the best course of action. Once agreed, the clinician will issue a prescription order.
With your consent, the clinician may also inform your doctor of the treatment prescribed. We recommend you agree to this, as your doctor is responsible for your overall care and should have a record of the consultation and any medication prescribed.
Your clinician may also take the opportunity to offer general health advice, including guidance on healthy living or stopping smoking.
Please note: Medication is not guaranteed and is provided only at the discretion of the assessing clinician.
What Happens After the Consultation?
After your consultation, you will receive a post-consultation notification summarising:
The outcome of your appointment
Any referrals made to your doctor
Any advice given by your clinician
Your family doctor is responsible for your overall care. Our clinicians will communicate with your doctor if they have concerns or recommendations that could affect your care. Referrals are only made with your explicit consent or where they form part of the terms of service you agreed to.
If a referral letter was issued, you can view a copy in the ‘Documents’ section of your account. If treatment was prescribed, it will appear in your Cart.
You may also receive a short survey about your experience. We encourage you to complete it. Your feedback helps us improve the service for you and other patients.
How to Complete Your Order After Treatment Is Prescribed
If your clinician prescribes treatment during the consultation, follow these steps to complete your order:
Go to your Cart. Use the account navigation to open your Cart.
Select ‘Checkout’. Proceed from the Cart to the checkout process.
Choose your delivery address. Select or add the address where you would like your medication delivered.
Choose your delivery method. Select from the available delivery options.
Confirm your billing address. Review and confirm your billing details.
Review your order. Check the order summary to make sure everything is correct.
Submit payment. Complete payment on our secure banking page. NowPatient never handles your payment details — all payments are processed securely by our banking partner.
Order confirmed. You will see an order confirmation screen and be redirected to your account homepage.
Reordering Your Medication
Fourteen days after receiving your first monthly supply, NowPatient will send you a notification advising that you are eligible to reorder. To reorder, you will need to navigate to the Get Treated Privately and select the option ‘Manage Treatments’. Here, you will be able to view the following sections:
Reorder
Voided
Pending
Select ‘Reorder’ and this will allow you to book a follow-up consultation.
For your own safety and for our prescribing guidelines, we do not issue more than 1 month supply at a time, this ensures your clinician can:
Follow up on your progress before issuing a new prescription
Assess any new information that may affect your current treatment plan
Confirm the treatment continues to remain safe, suitable, and effective
Adjust your dose if needed, or advise you to stop treatment
At the end of the follow-up, the clinician may advise you to stop treatment, stay on the current dose, or increase the dose. If it is safe to continue, the medication will be added to your Cart for checkout. As a responsible prescribing service, NowPatient always monitors treatment plans to ensure ongoing safety and suitability.
Your Prescribing Clinician
NowPatient’s prescribing clinicians are board-certified pharmacists, nurses, or doctors who can prescribe any medicine for any medical condition, subject to accepted accreditation and good clinical practice. Each clinician is registered with their respective regulatory body — for example, pharmacist independent prescribers in England are registered with the General Pharmaceutical Council (GPhC).
Every clinician undergoes an extensive background check, including a Disclosure and Barring Service (DBS) check, and a rigorous licence verification process. When you book, you will see the clinician’s full name, licence number, and any specialist credentials.
Our formulary of medications and conditions treated is controlled, governed, and continuously risk-assessed by our Medical Director, Dr. Ihtesham Sabri.
Please note: If your clinician does not prescribe what you were hoping for, it is because they have exercised their clinical judgement. NowPatient is a safe prescribing service, not a self-select service. If no prescription is issued, you will not be charged.
Medication Advice and Counselling
NowPatient’s pharmacists provide medication advice and counselling across all dispensing services. If you have any questions about your prescribed medication, our pharmacy team is available to help.
Delivery
Where Do You Deliver?
We deliver to all postcodes and zip codes worldwide. Some rural areas may experience slightly longer delivery times.
How Is My Order Packaged?
All orders are shipped in discreet, unmarked packaging, suitable for delivery to your home, workplace, or a neighbour’s address. For temperature-sensitive items (such as insulin or weight loss injections), we use cold chain-validated packaging to maintain product quality, safety, and efficacy.
First order restriction: For your protection, your first order can only be delivered to the address registered with NowPatient. Future orders can be delivered to any other address.
Delivery Options and Timescales
We aim to dispatch all orders placed Monday–Friday before 3pm on the same day. Orders placed after 3pm or on weekends are dispatched the next working day.
UK — Royal Mail Tracked 24 & Signed: Next-day delivery
Europe — Royal Mail Tracked: 3–5 working days
Worldwide — Royal Mail: 5–7 working days (tracked where available)
For deliveries outside the UK, check with your national postal service for accurate delivery days.
What If My Order Has Not Arrived?
You can check tracking details in the ‘Notifications’ section on your account homepage (click the bell icon) at any time after dispatch. If your delivery has not arrived within 10 days of the dispatch notification, contact us and we will do everything we can to resolve the issue.
Order Status Updates
NowPatient keeps you informed at every stage. You will receive status update notifications through:
Email
In-app notifications
Privacy, Security, and Data Protection
Are My Consultations Confidential?
Yes. NowPatient follows strict General Data Protection Regulations (GDPR) and is HIPAA compliant, ensuring Personal Health Information (PHI) is handled securely. Legal requirements ensure your personal data is managed with the utmost confidentiality. Records are maintained of all processing, and breaches are reported if they occur.
How Is My Data Protected?
NowPatient meets and exceeds UK and US data security standards, demonstrated through regular internal and external audits. Our externally audited accreditations include:
ISO27001
DTAC
DSPT
Cyber Essentials+
How Is My Data Stored?
Data residency is a key priority. UK-based data remains solely in the UK. US data is governed by HIPAA-prescribed data security protocols. The data centres we use align with the highest standards of security and privacy, safeguarded through regular external audits.
Are Remote Video Consultations Safe?
Yes. NowPatient has specific safeguards and protocols in place. Our video technology platform is certified to the highest industry standards of data security and clinical governance.
HOW IT WORKS
Order Delivery Guide


How will my order be delivered?
All orders are shipped in discreet and unmarked packaging, making them suitable for delivery to your home, workplace, or a neighbour. For your protection and safety, your first order can only be delivered to the address that is registered with NowPatient. Future orders can be delivered to any address you choose.
Where does NowPatient deliver?
NowPatient delivers to the UK, Europe, and worldwide. NHS services (such as NHS Online Pharmacy and NHS Pharmacy First) are available to patients in England only. Our private services and online pharmacy are available across the UK, with international shipping available to European and worldwide addresses. Please note that some remote or rural postcodes may experience slightly longer delivery times, and tracking availability for worldwide orders may vary depending on the destination country.
What delivery options are available?
UK orders are shipped via Royal Mail Tracked 24 & Signed, with next-day delivery as standard. European deliveries are sent via Royal Mail Tracked and typically arrive within 3–5 working days. Worldwide deliveries take 7–21 working days and are tracked where available in the destination country.
Delivery charges apply for most services. Shipping is included in the price for patients using our Get Treated Privately service in England, and is free for NHS Quit Smoking Service orders.
When will my order be dispatched?
We aim to dispatch all orders placed Monday to Friday before 3:00pm on the same working day. Orders placed after 3:00pm, or over weekends and bank holidays, will be dispatched on the next available working day.
Do you offer next-day delivery?
Yes. All UK orders are shipped via Royal Mail Tracked 24 & Signed, which delivers next day as standard. To qualify for same-day dispatch, please place your order before 3:00pm Monday to Friday. Orders placed after this time, or over weekends and bank holidays, will be dispatched on the next available working day.
Do you deliver temperature-sensitive or cold-chain medications?
Yes. We use a specialist courier service for all thermo-sensitive deliveries (such as insulin, GLP-1 weight loss injections like Mounjaro, and other refrigerated medications). Cold chain-validated packaging is used throughout the entire delivery process to ensure product quality, safety, and efficacy are always maintained.
How is cold-chain packaging handled?
Temperature-sensitive products are packed using validated cold chain packaging that maintains the required storage temperature throughout transit. Your parcel will normally receive an estimated delivery window from the courier on the day of delivery, so you can ensure someone is available to receive it. If you have concerns about receiving a cold-chain delivery, please contact our customer care team in advance.
Do you deliver controlled drugs?
Yes. Controlled drugs are delivered using a specialist courier service to ensure secure and compliant handling in accordance with UK regulations. These deliveries will always require a signature upon receipt.
How do I track my order?
Once your order has been dispatched, you will receive a dispatch notification containing your tracking details. You can also view your tracking information at any time in the 'Notification Feed' section on your account dashboard. Tracking is available for all delivery options.
Will I receive status updates about my order?
Yes. NowPatient uses a structured notification system to keep you fully informed throughout the order process. Every time your order status changes — from approval through to dispatch and delivery — you will be notified immediately. Notifications are sent via email and appear in the 'Notifications' section of your account homepage (accessible via the bell icon). This includes updates when your treatment is approved, dispensed, and shipped.
What order statuses will I see?
You can expect to see the following key status updates: Order Received, Prescription Approved (where applicable), Order Dispensed, Dispatched (with tracking reference), and Delivered.
Can I change my delivery address?
For your first order, delivery must be made to the address registered with NowPatient at the time of sign-up. This is a safety measure to verify your identity and protect your account. From your second order onwards, you can select from any saved address in your account or add a new delivery address during checkout.
Can I have my order delivered to my workplace or a neighbour?
Yes. From your second order onwards, you can have your medication delivered to any address, including your workplace, a family member's address, or a neighbour. All parcels are sent in discreet, unmarked packaging, so the contents will not be identifiable.
How do I update or add a new delivery address?
You can manage your delivery addresses directly within your NowPatient account settings. Additional addresses can also be added during the checkout process when selecting your delivery address. Simply select 'Add a new address' and enter the required details.
What should I do if my order hasn't arrived?
If you have not received your order within the expected delivery window, please first check your tracking details in the 'Notification Feed' section of your account dashboard. If after 10 days of dispatch you have still not received your delivery, please contact our customer care team and we will work to resolve the issue as quickly as possible.
What if my order arrives damaged?
If your order arrives in a damaged condition, please do not use the medication and contact our customer care team immediately. Please retain the original packaging and, if possible, take photographs of the damage, as this will help us raise a claim with the courier and arrange a replacement for you as quickly as possible.
My tracking shows delivered but I haven't received my parcel — what should I do?
First, check with any neighbours or safe locations at your property (such as a porch or outbuilding). If you still cannot locate your parcel, please contact our customer care team and we will investigate the matter with the courier on your behalf.
What happens if I miss my delivery?
If you miss a delivery, the courier will typically leave a card with instructions for rescheduling or collecting your parcel from a local depot. For cold-chain deliveries, it is particularly important to arrange redelivery promptly to maintain product integrity. If you have concerns about a missed cold-chain delivery, please contact our customer care team for guidance.
If you ship international, do I need to handle duties?
No. Our prices include customs duties, wherever you are located.
How are NHS repeat prescriptions delivered?
Once your GP has approved your prescription request, NowPatient's regulated online pharmacy will dispense and dispatch your medication. You will be notified at each stage of the process. NHS prescriptions are dispatched via Royal Mail Tracked 24 & Signed for next-day delivery, provided the order is placed before 3:00pm on a
working day.
Is delivery free for NHS prescriptions?
No. There is a small cost applied to all NHS prescription deliveries. This allows us to keep our service operational. NHS Quit Smoking Service orders qualify for free delivery. If you are using the Get Treated Privately service in England, shipping is included within the consultation and treatment price.
Can I specify a preferred delivery date for my NHS prescription?
At this time, NowPatient dispatches orders on the same working day if placed before 3:00pm Monday to Friday. All UK NHS prescriptions are sent via Royal Mail Tracked 24 & Signed for next-day delivery, so you can plan accordingly once you receive your dispatch notification.
How are private prescription medications delivered after a telehealth consultation?
Following your telehealth or video consultation, if a treatment is prescribed, it will be added to your cart automatically. After you complete checkout and payment, your order is sent to NowPatient's regulated online pharmacy for processing. You will receive status updates at every stage and your medication will be dispatched in discreet, unmarked packaging.
How quickly will I receive medication after my consultation?
If your consultation and checkout are completed before 3:00pm on a working day, we aim to dispatch your medication the same day. The total time to delivery will depend on the delivery method you select at checkout.
Is the packaging discreet?
Yes. All NowPatient orders are shipped in plain, unmarked packaging with no branding or indication of the contents on the outside. The packaging is suitable for delivery to your home, workplace, or a neighbour.
Will my parcel require a signature?
Yes. All UK orders are sent via Royal Mail Tracked 24 & Signed, which requires a signature upon delivery. Controlled drug deliveries will always require a signature regardless of the shipping method. For cold-chain deliveries, a signature is required to ensure someone is available to receive the medication promptly and maintain product integrity. For European and worldwide orders, signature requirements may vary depending on the destination country and the service available.
How do I contact NowPatient about a delivery issue?
You can reach our customer care team through the NowPatient website or app. Go to your account and use the Help or Contact Us section to raise a query. Our team is available to assist with any delivery-related concerns including missing parcels, tracking queries, or delivery address changes.
What are NowPatient's customer care hours?
Please visit the Contact Us section of the NowPatient website or app for up-to-date information on our customer care operating hours and available contact methods.
SAFE PRESCRIBING
Get Started With the Right Treatment for You
MEDICAL INFORMATION
Psoriasis Key Facts

(Current Version)
Psoriasis is a condition that appears as scaly patches on your skin and is thought to be caused by problems with the immune system. There is no specific cure for Psoriasis, but lifestyle changes can help manage the symptoms. Here, we will take a closer look at the causes, symptoms, types and treatment options available for Psoriasis.
What is Psoriasis?
Psoriasis is a skin disease thought to be caused by an overactive immune system, that results in the rapid growth and build up of skin cells. Psoriasis appears as plaque on the skin, most commonly between the ages of 15 and 25. It is not however contagious and can not be passed directly, from person to person.
Types of Psoriasis
There are many types of Psoriasis, each with its own symptoms, affecting different areas of the body.
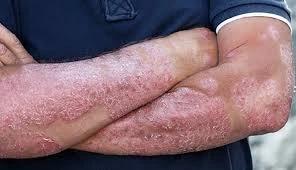
- Plaque Psoriasis: This is the most common type of Psoriasis, making up 80% of cases according to the American Academy of Dermatology. Symptoms include dry, red skin lesions covered in silver scales. Plaque Psoriasis may appear anywhere on your body but normally appears on the knees, elbows, scalp or lower back. In the most severe cases, skin may crack and bleed around the joints
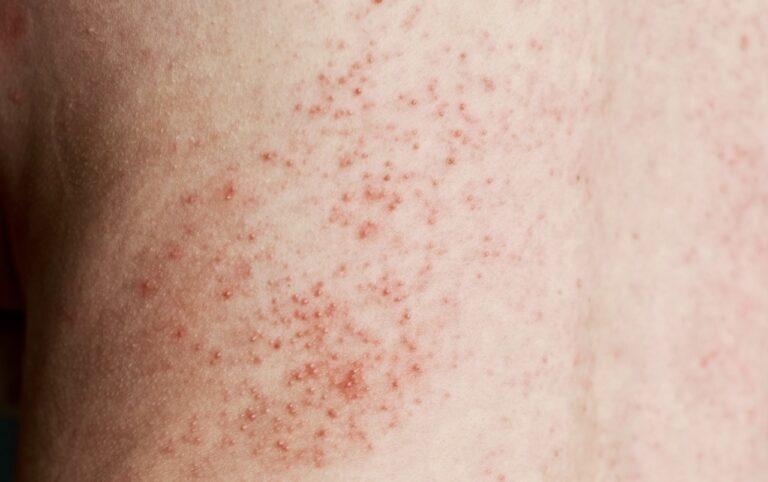
- Guttate Psoriasis: This appears as drop-shaped sores, less than 1cm, on your arms, legs, chest, or scalp. Some people may develop plaque Psoriasis. Guttate Psoriasis may occur after a strep throat infection and is more prevalent in children, teenagers and young adults
- Pustular Psoriasis: Characterized by pus-filled blisters surrounded by red skin, primarily affecting the hands and feet. Pustular Psoriasis is a rarer type of Psoriasis. Different types of pustular Psoriasis affect different parts of the body
- Inverse Psoriasis: These appear as large smooth red patches in skin folds, beneath the armpits, breasts, between the buttocks or groin. This is made worse by sweating and friction
- Erythrodermic Psoriasis: A rare and severe form of Psoriasis that covers large areas of the body and requires immediate medical attention. Erythrodermic Psoriasis causes discolouration of the skin and the shedding of scales on sheets. It may be triggered by bad sunburn, certain medications, infections, and stopping Psoriasis treatment
- Scalp Psoriasis: This can occur on all or part of the scalp. Symptoms may include red patches of skin with thick silvery-white scales. Scalp Psoriasis can feel extremely itchy, or cause no discomfort at all. In more serious cases it can cause hair loss. This, however, is usually only temporary
- Nail Psoriasis: Nail Psoriasis affects about half of all people with Psoriasis, causing your nails to become discoloured, develop tiny dents or pits, or grow abnormally. Nails can become loose and detach from your nail bed. In more severe cases, your nails may crumble
- Palmoplantar Pustular Psoriasis causes pustules to appear on the palms of your hands and the soles of your feet. They appear as circular brown, scaly spots, which peel off
- Acropustulosis: Pustules appear on your fingers and toes, then burst, leaving bright red areas, which may ooze or become scaly. Acropustulosis may also lead to painful nail deformities
- Erythrodermic Psoriasis is a rare type of Psoriasis, affecting nearly all the skin on your body. It causes intense itching or burning and can also cause you to lose fluids and proteins, causing you to develop infections, dehydration, malnutrition, hypothermia and heart disease
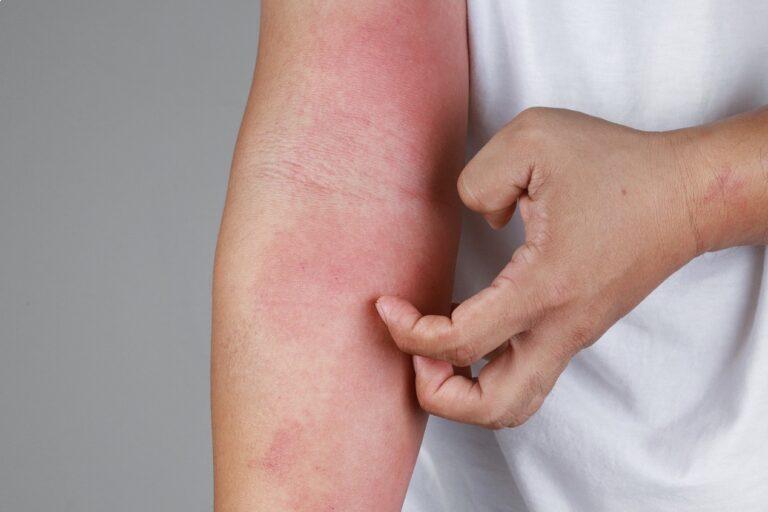
Symptoms of Psoriasis
Symptoms can vary based on the individual and the type of Psoriasis. Symptoms include:
- Inflamed patches of skin covered in scales
- Itching, burning, or stinging
- Dry, cracked skin that may bleed
- Nail abnormalities, such as pitting or ridges
- Joint pain and stiffness
Symptoms range from mild to severe and may come and go in cycles. Speak to a healthcare professional for a diagnosis and an appropriate treatment plan.
Causes of Psoriasis
Psoriasis is classed as an autoimmune disease. The exact trigger is not fully understood, but it is thought that genetics and environmental factors play a major role.
- Genetics: Family history of Psoriasis increases the likelihood of developing the condition. Certain genes related to immune system function are thought to contribute to the development of Psoriasis
- Immune system dysfunction: In individuals with Psoriasis, the immune system mistakenly attacks healthy skin cells, leading to inflammation and rapid cell turnover
- Environmental factors: Infections, such as streptococcal infections, can trigger or exacerbate Psoriasis symptoms. Other factors, such as stress, skin injuries, smoking, and obesity, may also contribute to the development or worsening of Psoriasis
- Other medications: Beta blockers, other high high blood pressure drugs, antimalarials, lithium and other mood stabilizers, NSAIDs and antibiotics
Who is at risk?
Certain factors may increase the risk of developing Psoriasis and flare-ups. These include:
- A family history of Psoriasis
- Age, with it being most common between the ages of 15 and 25
- Psoriasis is more common in certain ethnic groups, with higher rates in those of European descent
- Smoking, obesity, and certain medications can all increase the risk of developing Psoriasis
Diagnosing Psoriasis
Your healthcare provider will carry out a physical examination and review your medical history. They may also carry out a skin biopsy to confirm your diagnosis. You should let your healthcare provider know about any family history of Psoriasis, or of any other risk factors that make your symptoms worse.
Treatment options for Psoriasis
The choice of treatment will depend on the type of Psoriasis and how severe it is, as well as age, general health, and personal preferences. Mild Psoriasis can be treated with creams or ointments such as Fucibet or Dermovate, while moderate and severe Psoriasis may need treatment with tablets, injections, or phototherapy. Treatment options include:
- Topical treatments: Vitamin D creams, topical corticosteroid (steroid) ointments, and lotions containing retinoids (vitamin A derivative) applied directly to the affected skin to reduce inflammation and promote healing
- Phototherapy (light therapy): Controlled exposure to ultraviolet light to slow down skin cell turnover and reduce inflammation. Psoralen plus ultraviolet-A radiation (PUVA) combines psoralen with ultraviolet light
- Systemic medications: Prescription medications that target the immune system, (such as methotrexate, acitretin) and reduce inflammation throughout the body
- Biologics and small molecule inhibitors: Advanced therapies (etanercept, adalimumab) that specifically target molecules involved in the immune response, providing targeted relief from Psoriasis symptoms
- Lifestyle modifications: Adopting healthy habits, such as managing stress, maintaining a healthy weight, and avoiding Psoriasis triggers, can help improve symptoms and overall well-being
It is important to work closely with a healthcare provider to develop an individualized treatment plan that best suits your needs.
Lifestyle changes for Psoriasis management
In addition to medical treatments, certain lifestyle changes can help manage Psoriasis symptoms and improve overall well-being. These include:
- Moisturizing the skin
- Avoiding common triggers
- Practicing good skin hygiene
- Maintaining a healthy weight
- Managing stress
- Protecting the skin from excessive sun exposure
Psoriasis and mental health
The nature of the condition can lead to embarrassment, self-consciousness, and low self-esteem and people with Psoriasis may be at a higher risk of mental health conditions. It is important to seek support from mental health counselors or support groups.
Psoriasis and Psoriatic Arthritis
Up to a third of people with Psoriasis will develop psoriatic arthritis. Symptoms include inflammation, pain, and stiffness in the joints, as well as skin and nail changes.
Treatment options include medications to reduce the inflammation, physical therapy and lifestyle modifications, and a combination of dermatologists, rheumatologists, and other healthcare providers is often needed to manage both conditions effectively.
Conclusion
By understanding the causes, types, symptoms and treatment options available for Psoriasis, individuals can develop plans to manage this skin condition.
If you think you have Psoriasis and its associated symptoms, speak to your doctor for a diagnosis and advice on the most appropriate treatment for your condition.
Sources
- NHS Psoriasis
- WebMD – Psoriasis
- Cleveland Clinic – Psoriasis guide
- Psoriasis.org – About Psoriasis
- NIH – Psoriasis
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.
Related Articles
OUR CUSTOMERS VIEW
What Customers Love About Our Service
We want everyone to be happy and healthy, that’s what keeps us going. Read what some of them have to say about us.
Medicines Experts
Meet Our Medical Team
We are a broad skilled and passionate group of clinicians with experience of operating in regulated health systems in the United Kingdom & United States. Providing excellent care and advice is at the heart of everything we do. You can read more about our medical team by visiting the medical team page or learn more about how we curate content by visiting our editorial process