Crohns Disease
Get valuable insights into Crohns Disease, including its causes, symptoms, prevention strategies, and treatment options, while also learning about how you can lower the cost of the medications used to treat Crohns Disease.

MEDICAL INFORMATION
Crohns Disease Key Facts
Related Medications
Crohn’s disease is a type of inflammatory bowel disease (IBD) that affects millions of people worldwide. This comprehensive article aims to provide an overview of Crohn’s disease, including its symptoms, causes, diagnostic methods, and available management strategies.
What is crohn’s disease?
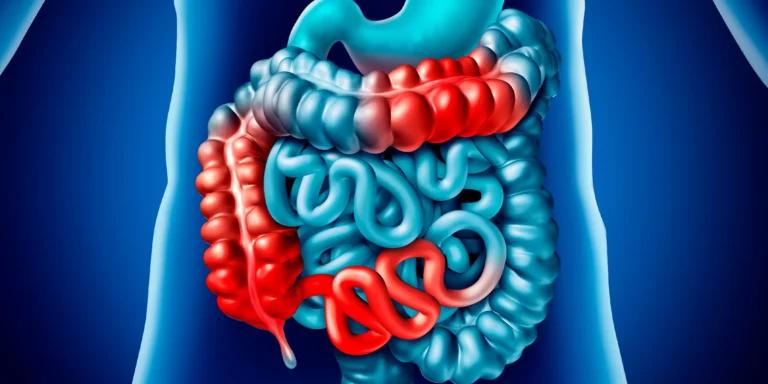
Crohn’s disease is an inflammatory condition that primarily affects the gastrointestinal tract, causing chronic inflammation and damage to the digestive system. It can affect any part of the digestive tract from the mouth to the anus, but it most commonly affects the small intestine and the beginning of the large intestine.
What are the symptoms of crohn’s disease?
Crohn’s disease is a chronic inflammatory bowel disease that can affect any part of the gastrointestinal tract. The symptoms can vary in severity and may fluctuate over time. Here are some common symptoms associated with Crohn’s disease:
Abdominal pain and cramping
Persistent or intermittent abdominal pain and cramping are common symptoms of Crohn’s disease. The pain may be localized or spread across the abdomen, and it can range from mild to severe.
Diarrhea
Frequent loose stools or diarrhea is another hallmark of crohn’s disease symptoms. The stools may be watery, contain mucus or blood, and may be accompanied by an urgent need to have a bowel movement.
Rectal bleeding
Blood in the stool or visible rectal bleeding may occur due to inflammation and ulceration of the intestinal lining. It can range from mild to severe and may vary in color, from bright red to dark, tarry stools.
Fatigue and weakness
Chronic inflammation and nutrient malabsorption can lead to fatigue and a general feeling of weakness. This can be exacerbated by anemia resulting from reduced iron absorption.
Unintended weight loss
Reduced appetite, malabsorption of nutrients, and increased metabolic demands due to inflammation can lead to unintended weight loss in individuals with Crohn’s disease.
Loss of appetite
Many individuals with Crohn’s disease experience a decreased appetite, which can contribute to weight loss and nutritional deficiencies.
Fever
Fever is a common symptom during active periods of inflammation and can be accompanied by other flu-like symptoms.
Joint pain
Crohn’s disease can cause inflammation in joints, leading to pain, stiffness, and swelling. This is known as arthritis or arthralgia.
Abscesses
In patients with Crohn’s disease, abscesses, or collections of pus, often develop in the abdomen, pelvis, or around the anal area.
Skin problems
Some individuals with Crohn’s disease may experience skin problems, such as rashes, ulcers, or sores, due to inflammation or complications of the disease.
It’s important to note that not everyone with Crohn’s disease will experience all of these symptoms. Additionally, symptoms can vary depending on the location and severity of inflammation within the gastrointestinal tract. If you are experiencing persistent gastrointestinal symptoms or suspect you may have Crohn’s disease, it is important to seek medical evaluation and diagnosis from a healthcare professional.
Anal fissures
Anal fissures are relatively common in Crohn’s disease. An anal fissure usually presents as a tear or sore which develops in the skin around the anus and the anal canal.
Inflammation
About a third of Crohn’s patients have inflammation exclusively in the ileum, the deepest part of the small bowel.The inflammation of the ileum, caused by Crohn’s disease, is called Ileitis. Crohn’s disease causes inflammation.
What are the causes and risk factors for crohn’s disease?
The exact cause of Crohn’s disease remains unknown, but several factors are believed to contribute:
- Genetic predisposition
- Abnormal immune response
- Environmental factors
- Dysbiosis of gut microbiota
How is crohn’s disease diagnosed?
Diagnosing Crohn’s disease involves a combination of medical history assessment, physical examination, laboratory tests, imaging studies, and sometimes tissue biopsies. Here are the common diagnostic methods used for Crohn’s disease:
Medical history assessment
The healthcare provider will gather information about your symptoms, their duration, and any family history of inflammatory bowel disease. They will also inquire about factors like diet, lifestyle, and medication history.
Physical examination
A physical examination by a gastroenterologist who specializes in inflammatory bowel disease, may be conducted to check for signs of inflammation, abdominal tenderness, and other related symptoms. The healthcare provider may also perform a digital rectal examination to assess for any abnormalities in the rectum and anus.
Laboratory tests
Various laboratory tests may be conducted to assist in the diagnosis and assessment of Crohn’s disease, including:
- Blood tests: These may include complete blood count (CBC) to check for anemia, C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) to measure inflammation levels, and liver function tests
- Stool tests: These tests help identify the presence of blood, infections, or inflammation in the digestive tract
Imaging studies
Imaging techniques are used to visualize the digestive tract and identify any abnormalities or signs of inflammation. Common imaging studies include:
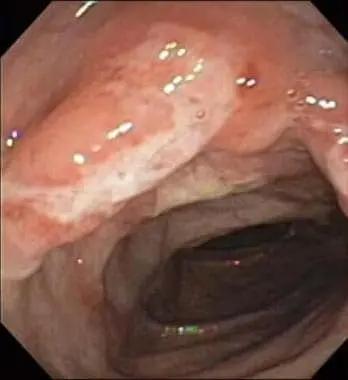
- Endoscopy: This includes procedures like upper endoscopy (esophagogastroduodenoscopy) and colonoscopy, where a flexible tube with a camera is used to examine the esophagus, stomach, small intestine, and colon
- Imaging scans: X-rays, computed tomography (CT), magnetic resonance imaging (MRI), or capsule endoscopy may be employed to visualize different parts of the digestive tract
- CT enterography is a special CT scan that is better able to visualize the small intestine
Tissue biopsies
During endoscopic procedures, the healthcare provider may take small tissue samples (biopsies) from affected areas for microscopic examination. Biopsies can help confirm the presence of inflammation, assess disease severity, and differentiate Crohn’s disease from other conditions.
Barium swallow
Barium, which is a metallic, chalky, liquid is used to coat the inside of organs so that they will show up on an X-ray, when swallowed. A barium X-ray can show where the Crohn’s disease is and how severe it is. It is especially useful for finding any problems in parts of the small intestine that can’t be easily viewed by other techniques
Differential diagnosis
It is important to differentiate Crohn’s disease from other conditions that may cause similar symptoms. This may involve ruling out infections, other types of inflammatory bowel disease (such as ulcerative colitis), irritable bowel syndrome (IBS), or other gastrointestinal disorders.
What are the treatment and management options for crohn’s disease?
The treatment of Crohn’s disease aims to reduce inflammation, control symptoms, achieve and maintain remission, and improve the quality of life for individuals. The specific treatment modalities may vary depending on the severity of the disease, the location of inflammation, and the individual’s response to different therapies. Here are some common treatment options for Crohn’s disease:
Medications
- Anti-inflammatory drugs: Aminosalicylates (5-ASA), such as mesalamine, may be used to reduce inflammation in mild to moderate cases
- Corticosteroids: These medications, like prednisone or budesonide, are used to reduce inflammation during flare-ups but are generally not recommended for long-term use due to their potential side effects
- Immunomodulators: Medications like azathioprine, mercaptopurine, or methotrexate may be prescribed to suppress the immune system and reduce inflammation
- Biologic therapies: Drugs such as anti-tumor necrosis factor (TNF) agents (e.g., infliximab, adalimumab) and other biologics (e.g., vedolizumab, ustekinumab) target specific molecules involved in inflammation and can induce and maintain remission in moderate to severe cases
Nutritional therapy
- Exclusive enteral nutrition (EEN): This involves consuming a liquid formula as the sole source of nutrition for a specific period. EEN can help reduce inflammation and promote healing, especially in children and adolescents
- Partial enteral nutrition: In this approach, a combination of normal food and nutritional supplements is used to supplement the diet and provide additional nutrients
Surgery
Surgery may be necessary in certain cases, such as:
- Strictureplasty: Widening of narrowed sections of the intestine to relieve blockages
- Intestinal resection: Removal of the affected segment of the intestine
- Fistula repair: Closure of abnormal passages that form between different parts of the intestine or between the intestine and other organs
Symptom management
- Anti-diarrheal medications: Medications such as loperamide can help control diarrhea
- Pain relievers: Over-the-counter pain medications or prescription options may be used to alleviate abdominal pain or cramping
- Iron supplements: These may be prescribed to address anemia resulting from chronic bleeding or malabsorption
Lifestyle modifications
- Dietary adjustments: Identifying and avoiding trigger foods that exacerbate symptoms, such as high-fiber foods, spicy foods, and dairy products, can help manage symptoms
- Stress management: Stress reduction techniques, such as relaxation exercises, counseling, or mindfulness practices, may help minimize flare-ups
It’s important to note that the treatment approach should be individualized based on the specific needs and response of each person with Crohn’s disease. Regular follow-up with healthcare professionals and adherence to treatment plans are crucial for managing the condition effectively.
What medications are used in crohn’s disease?
Aminosalicylates (5-ASA)
- Mesalamine (also known as mesalazine)
- Sulfasalazine
- Balsalazide
Corticosteroids
- Prednisone
- Budesonide
- Hydrocortisone
- Methylprednisolone
Immunomodulators
- Azathioprine
- 6-Mercaptopurine (6-MP)
- Methotrexate
- Cyclosporine
Biologic Therapies
Anti-tumor necrosis factor (TNF) agents
- Infliximab
- Adalimumab
- Certolizumab pegol
- Golimumab
Integrin receptor antagonists
- Vedolizumab
- Natalizumab
Interleukin-12/23 inhibitors
- Ustekinumab
Janus Kinase (JAK) Inhibitors
- Tofacitinib
Antibiotics
- Metronidazole
- Ciprofloxacin
- Rifaximin
Coping with crohn’s disease
Living with Crohn’s disease can be challenging, but several strategies can help individuals cope with the condition:
- Seek support from healthcare professionals, support groups, or therapists
- Maintain open communication with loved ones and educate them about the disease
- Make necessary lifestyle adjustments to minimize triggers and manage stress levels
- Stay informed about the latest research and treatment options
What crohn’s disease support organizations are there available to support me in the UK?
- Crohn’s & Colitis UK: Crohn’s & Colitis UK is the leading charity organization in the UK dedicated to supporting individuals with Crohn’s Disease, ulcerative colitis, and other forms of inflammatory bowel disease (IBD). They offer information resources, support services, a helpline, local support groups, and an online community
- The IBD Registry: The IBD Registry is a national organization that focuses on improving the care and treatment of individuals with IBD, including Crohn’s Disease. They collect data, conduct research, and collaborate with healthcare professionals to enhance understanding and support for IBD patients
- St Mark’s Hospital Foundation: St Mark’s Hospital is a renowned center for bowel disease treatment and research. The St Mark’s Hospital Foundation supports patients by providing information resources, patient support groups, and access to specialized care
- Guts UK: Guts UK is a charity organization that supports research, raises awareness, and provides information on various digestive disorders, including Crohn’s Disease. They offer resources, research updates, and a helpline to assist individuals in understanding and managing their condition
What crohn’s disease support organizations are there available to support me in the US?
- Crohn’s & Colitis Foundation: The Crohn’s & Colitis Foundation is a national non-profit organization dedicated to supporting individuals with Crohn’s Disease, ulcerative colitis, and other forms of inflammatory bowel disease (IBD). They offer education resources, support groups, advocacy initiatives, research funding, and a helpline
- United Ostomy Associations of America (UOAA): The UOAA is an organization that supports individuals with ostomies, including those resulting from Crohn’s Disease. They provide resources, educational materials, support groups, and advocacy for individuals living with IBD and ostomies
- Crohn’s & Colitis Community: The Crohn’s & Colitis Community is an online community and resource center that provides support, information, and a platform for individuals affected by Crohn’s Disease and ulcerative colitis. They offer forums, educational materials, and a community network
- ImproveCareNow: ImproveCareNow is a collaborative network of healthcare providers, researchers, and patients focused on improving care for children and adolescents with Crohn’s Disease and ulcerative colitis. They provide resources, research updates, and opportunities for patient engagement
- IBD Support Foundation: The IBD Support Foundation is a non-profit organization that offers resources and support for individuals with Crohn’s Disease and ulcerative colitis. They provide educational materials, support groups, financial assistance programs, and an online community
Summary
Crohn’s disease is a chronic inflammatory bowel disease that can significantly impact a person’s quality of life. While the exact cause remains unknown, advancements in understanding and treatment options have improved the management of this condition. Early diagnosis, appropriate medical care, and lifestyle modifications can help individuals with Crohn’s disease lead fulfilling lives. If you suspect you may have Crohn’s disease or are experiencing related symptoms, it is crucial to consult with a healthcare professional for accurate diagnosis and guidance. In addition patients with ulcerative colitis and Crohn’s disease should have regular screenings for colon cancer, due to being at higher risk than the wider general population.
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.