Osteoporosis Symptoms Causes and Treatment

Osteoporosis affects over 3 million people in the UK and is caused by a loss of bone density. It can be a debilitating disease leading to serious health complications, including bone fractures and immobility. In this article we’ll take a closer look at the causes, symptoms and treatment options for osteoporosis.
What is Osteoporosis?
Osteoporosis is a condition characterised by low bone mass and deterioration of bone tissue. This leads to bones that are weak and porous and more susceptible to the risk of fracture. While osteoporosis can affect people of all ages, it is most common in older adults post-menopause. In fact, one in two women over 50 years of age will suffer from osteoporosis or low bone mass in their lifetime. Men can also develop osteoporosis, but at a much lower rate. About one in four men over the age of 50 will develop the condition.
How does bone-building in the body work?
Everybody knows that bones are important. They provide structure for the body, protect vital organs and allow us to move. But what many people don’t realise is that bones are constantly changing. The bone-building cycle is a continuous process that helps to keep bones healthy and strong.
The first step in the cycle is called osteogenesis or the formation of new bone tissue. This process begins in childhood and continues into adolescence when the skeleton is growing and bones are being laid down at a rapid pace. Once the skeleton has reached its full adult size, osteogenesis slows down but doesn’t stop completely. Even in adults, small amounts of new bone tissue are always being formed.
The second step in the cycle is called resorption, or the breakdown of old bone tissue. This process occurs throughout life and helps to remove damaged or worn-out bone cells. Resorption also makes room for new bone cells to be formed during osteogenesis.
The balance between osteogenesis and resorption is crucial for maintaining strong healthy bones. If this balance is disrupted, it can lead to problems such as osteoporosis, a condition where bones become weak and fragile. However, by understanding how the bone-building cycle works, we can take steps to protect our skeletons and keep our bones healthy for life.
What are the causes of osteoporosis?
There are numerous factors that can increase your risk of developing osteoporosis. Some of the most common include:
- Gender: Women are far more likely than men to develop osteoporosis. In fact, nearly 80% of all people with osteoporosis are women. Post-menopausal women are particularly at risk because they experience a decrease in estrogen levels which can lead to bone loss. Other risk factors for women include amenorrhea (absence of menstrual periods), early menopause (before age 45) or they’ve had their ovaries removed
- Age: Osteoporosis risk increases with age because bone loss occurs more rapidly as we age. Age-related bone loss begins around age 35 in women and around age 40 or 50 in men
- Family history of osteoporosis or hip fractures: If you have a close relative with osteoporosis or hip fractures (i.e. parent or sibling), your risk for developing the condition is increased
- Lifestyle factors: Smoking, excess alcohol consumption, lack of exercise and a poor diet low in calcium and vitamin D can increase your risk for osteoporosis and fractures
- Medical conditions: People with certain medical conditions such as rheumatoid arthritis, Crohn’s disease, celiac disease, overactive thyroid, anorexia nervosa, eating disorders, Cushing’s syndrome, hyperthyroidism, or cancer are at increased risk for developing osteoporosis
- Medications: Certain medications can increase your risk for developing osteoporosis. These include corticosteroids, anticonvulsants, heparin, activity suppressors and gonadotropin inhibitors. Treatments for prostate cancer that reduce testosterone levels in men and treatments for breast cancer that reduce estrogen levels in women are likely to accelerate bone loss
- Radiation therapy: People who have undergone radiation therapy have an increased risk of developing osteoporosis
- Small frame: Individuals who have small bone frames are more prone to osteoporosis
- Body weight: People who weigh less and have less muscle are more at risk for this condition
- Ethnicity: Caucasians and Asians are at greater risk for developing osteoarthritis
People with these risk factors should consider talking to their doctor about ways to prevent or delay osteoporosis.
What are the symptoms of osteoporosis?
Osteoporosis often develops without any symptoms which is why it’s important to be aware of your risks and get screened if necessary. Bone density loss happens gradually over time, so by the time symptoms do develop, the disease is often quite advanced.
There are a number of symptoms associated with osteoporosis, including:
- Bone pain: This can range from mild discomfort to severe pain that limits your ability to move
- Stooped posture: As the bones weaken, they may start to crumble, causing the spine to curve and giving you a stooped posture
- Height loss: Bones may shrink in size due to osteoporosis, resulting in a loss of height over time
- Fractures: Osteoporosis makes bones fragile and more likely to break. A fracture can occur with even a minor fall or bump
- Change in appearance: As osteoporosis progresses, you may notice changes in the shape of your fingers and hands, as well as other parts of your body. The skin may also thin and become bruised easily
How is osteoporosis diagnosed?
In order to diagnose osteoporosis, your doctor will first ask about your personal and family medical history. They will also perform a physical exam, paying special attention to your spine, ribs and hips.
Dual-energy X-ray absorptiometry (DEXA) is a bone density test that can help your doctor determine if you have osteoporosis. This test measures your bone mineral density, which is the amount of minerals in your bones. The DEXA scan uses two different energy levels of X-rays to measure your bone density. The results of the test are called T-scores. A T-score of -1 or above is considered normal. A T-score between -1 and -2.5 indicates low bone density, or osteopenia. A T-score of -2.5 or below indicates osteoporosis. If you have a T-score of -2.5 or below, you may be at increased risk for fractures. DEXA scans are painless and take about 15 minutes to complete. Talk to your doctor about whether a DEXA scan is right for you.
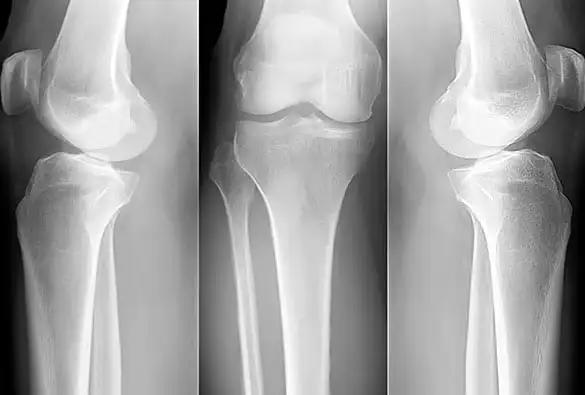
Another way to diagnose osteoporosis is to look for signs of fractures. This can be done with X-rays, but sometimes fractures can only be seen on MRI or CT scans. Finally, blood tests can sometimes be helpful in diagnosing osteoporosis. These tests measure levels of calcium, vitamin D and other minerals that are important for bone health.
How do you treat osteoporosis?
The best approach to osteoporosis treatment depends on a number of factors, including the severity of the condition, the underlying cause and the patient’s age and health. In general however, treatment for osteoporosis focuses on two main goals: preventing further bone loss and reducing the risk of fractures.
There are a number of different medications that can be used to achieve these goals. Medications used to treat osteoarthritis include bisphosphonates (such as Fosamax), denosumab (Prolia), estrogen therapy, selective estrogen receptor modulators (SERMs) (such as Evista), parathyroid hormone therapy (Forteo) and calcitonin salmon (Miacalcin). Calcium supplements and vitamin D supplements are also frequently recommended, as they can help to improve bone density. In some cases, it may also be necessary to take medication to regulate hormone levels or reduce inflammation.
There are several things you can do to keep healthy bones as you age:
- Healthy diet: Get enough calcium and vitamin D: Calcium is essential for strong bones and vitamin D helps your body absorb calcium. Good sources of calcium include dairy products, leafy green vegetables, sardines and calcium-fortified foods. You can get vitamin D from sunlight, food and supplements
- Regular exercise: Weight-bearing exercise helps to keep bones strong. Walking, running, stair climbing and lifting weights are all good exercises for bone health
- Don’t smoke: Smoking increases your risk of osteoporosis. If you smoke, talk to your doctor about ways to quit
- Limit alcohol intake: Drinking too much alcohol can also increase your risk of osteoporosis. If you drink alcohol, do so in moderation
- Avoid any exercise that presents a risk of falling. Also, do not do high-impact exercises that can cause fractures in older adults
- Remove household hazards, such as throw rugs, to reduce the risk of falls
By taking these steps, you can help keep your bones healthy as you age and reduce your risk of developing osteoporosis.
What is a Vertebral Compression Fracture?
People with osteoporosis or other conditions that affect bone strength are at greater risk for developing vertebral compression fractures.
A vertebral compression fracture is a type of osteoporotic fracture that occurs when the vertebrae (the bones of the spine) collapse. This can cause the spine to lose its normal shape and can lead to pain, deformity and disability.
There are different degrees of VCFs. A mild VCF may only involve a slight collapse of the vertebrae, while a more severe VCF can cause the vertebrae to collapse completely. Symptoms of a VCF can include back pain or neck pain, loss of height and a stooped posture. If you think you may have a VCF, it’s important to see your doctor right away for an evaluation and treatment. Treatment options may include non-steroidal anti-inflammatory drugs (NSAIDs), osteoporosis medications, braces and/or surgery. With proper treatment, most people with VCFs can experience significant pain relief and prevent further vertebral collapse.
What is the difference between osteoporosis and osteopenia?
Osteopenia and osteoporosis are often mentioned together because they are both bone diseases. While osteopenia is a bone condition characterised by lower-than-normal bone density, osteoporosis is a more serious condition that leads to thinning of the bones and an increased risk of fractures. People with osteopenia have a higher risk of developing osteoporosis, but not all people with osteopenia will go on to develop osteoporosis. Treatment for osteopenia is typically focused on lifestyle changes and dietary modifications, while treatment for osteoporosis may also include medications to help improve bone density.
Osteoporosis is a serious condition that can cause debilitating health problems. By treating osteoporosis early, you have the best chance of avoiding broken bones as you get older. If you think you may be at risk for developing osteoporosis or are experiencing any symptoms described above, please make an appointment with your doctor or healthcare provider who can complete an osteoporosis risk assessment.
Sources
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.