Athlete’s Foot Causes, Symptoms and Treatments

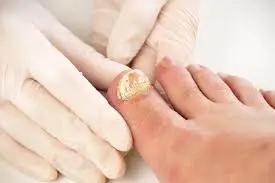
Athlete’s foot, also known as tinea pedis, is a common fungal skin infection that primarily affects the feet. It is characterized by itchy, scaly, and sometimes cracked skin, especially between the toes. This condition is highly contagious and can spread through contact with infected surfaces or through direct contact with an infected person. In this comprehensive guide, we will explore the causes, symptoms, and effective treatments for athlete’s foot.
Causes of Athlete’s Foot
Athlete’s foot is caused by a group of fungi known as dermatophytes, which thrive in warm and moist environments. These fungi can be found on floors, towels, and shoes, making it easy for them to spread. Certain risk factors increase the likelihood of developing athlete’s foot, including:
- Excessive sweating: People who sweat heavily are more prone to athlete’s foot, as the excessive moisture provides an ideal environment for fungal growth
- Wearing enclosed footwear: Tight-fitting shoes trap moisture, creating a breeding ground for fungi
- Sharing personal items: Sharing items such as towels, socks, or shoes with someone who has athlete’s foot can increase the risk of infection
- Walking barefoot in public areas: Walking barefoot in communal areas like locker rooms, saunas, and swimming pools exposes your feet to fungi
- Compromised immune system: Individuals with weakened immune systems, such as those with diabetes or HIV, are more susceptible to fungal infections
Symptoms of Athlete’s Foot
The area between the toes is most often affected, but the infection may spread to the soles of the feet or to the toenails. Athlete’s foot symptoms can vary from person to person, but they generally include:
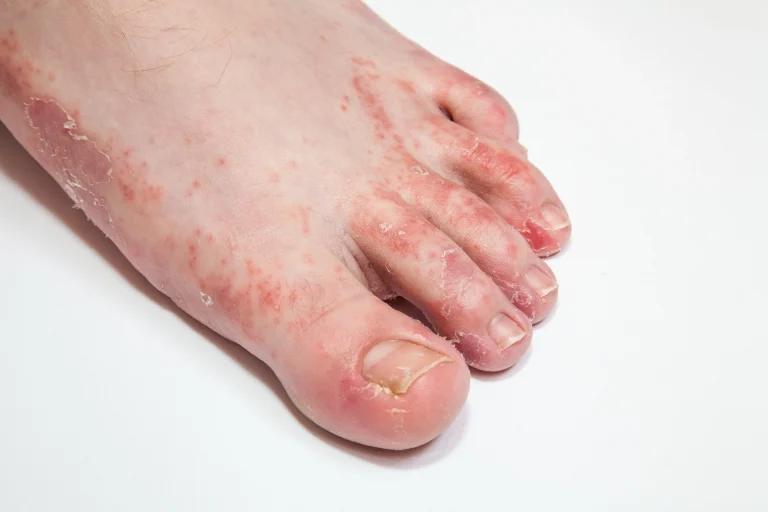
- Itchy, scaly rash: Athlete’s foot often begins as an itchy, scaly rash between the toes. The affected skin may appear white and can sometimes become cracked or bleed
- Burning or stinging sensation: Many individuals with athlete’s foot experience a burning or stinging sensation, particularly after removing their shoes and socks
- Inflammation: The skin affected by athlete’s foot may become inflamed, appearing reddish, purplish, or grayish, depending on the individual’s skin color
- Blisters: In some cases, athlete’s foot can lead to the formation of fluid-filled blisters, which can be painful and may break open
- Dry, scaly skin: Athlete’s foot can cause dry, scaly skin on the bottom of the foot that extends up the sides
If you suspect you have athlete’s foot and it does not improve within two weeks of self-treatment with over-the-counter antifungal products, it is advisable to consult a healthcare professional. Additionally, individuals with diabetes or signs of infection, such as swelling, pus, or fever, should seek medical attention promptly.
Diagnosis of Athlete’s Foot
In most cases, healthcare professionals can diagnose athlete’s foot based on a physical examination of the affected area. They may examine the appearance of the rash and inquire about symptoms. In certain situations, they may also collect a skin scraping or use a specialised light called a Wood’s lamp to confirm the presence of fungi.
Effective treatments for Athlete’s Foot
Thankfully, athlete’s foot can be effectively treated with various over-the-counter and prescription antifungal medications. These treatments can come in the form of creams, ointments, gels, sprays, or powders. The active ingredients commonly found in these products include clotrimazole, miconazole, tolnaftate, terbinafine, fluconazole, itraconazole, and others.
When using antifungal medications, it is crucial to follow the instructions carefully and complete the full course of treatment. Discontinuing treatment prematurely may result in the return of the infection, which can be more challenging to treat. In addition to antifungal medications, several self-care measures can help alleviate symptoms and prevent the recurrence of athlete’s foot:
- Keep your feet clean and dry: Wash your feet daily with warm, soapy water and thoroughly dry them, especially between the toes
- Use topical antifungal creams, powders or sprays: Applying an over-the-counter antifungal powder, cream or spray to your feet, particularly if you are prone to athlete’s foot, can help prevent recurrence
- Wear moisture-wicking socks: Choose socks made from breathable materials, such as cotton socks, that help keep your feet dry. Avoid wearing nylon socks, as they can trap moisture
- Alternate shoes: Give your shoes time to dry out by alternating between different pairs. This helps prevent the accumulation of moisture
- Protect your feet in public areas: Wear shoes or waterproof sandals, such as flip-flops, in public areas like swimming pools, locker rooms, and public showers
- Avoid sharing personal items: Do not share towels, socks, or shoes with others to minimise the risk of spreading the infection
It is essential to continue practising good foot hygiene and taking preventive measures even after the symptoms disappear to prevent a recurrence of athlete’s foot.
Complications and when to seek medical attention
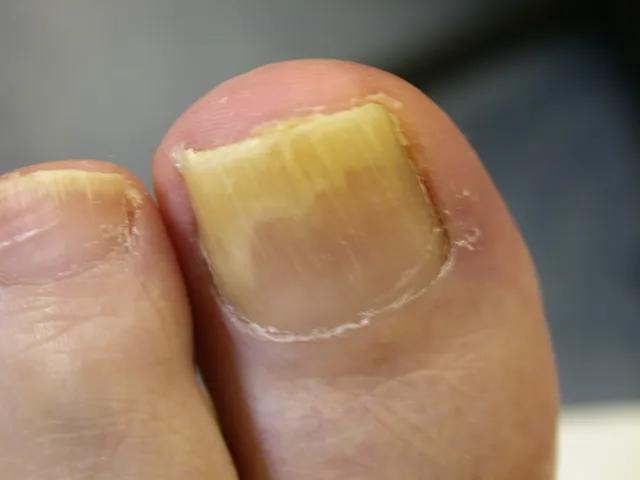
While athlete’s foot is generally a mild and self-limiting condition, it can lead to complications if left untreated. If the infection spreads to other parts of the body, such as the groin, it can result in jock itch, another fungal infection. Additionally, the fungus can invade the toenails, causing a fungal nail infection that is more challenging to treat.
If over-the-counter treatments are ineffective, or if you experience severe discomfort, persistent symptoms, or signs of a more serious infection, it is recommended to consult a healthcare professional. This is particularly important for individuals with underlying health conditions such as diabetes or a weakened immune system.
Preventing Athlete’s Foot
Prevention plays a crucial role in reducing the risk of athlete’s foot. Here are some preventive measures you can take:
- Keep your feet dry: Dry them thoroughly, especially between the toes, after washing them. Avoid wearing damp socks or shoes
- Choose appropriate footwear: Opt for shoes made from breathable materials that allow air circulation and minimize moisture build-up
- Wear moisture-wicking socks: Select socks made from materials like cotton that help absorb moisture and keep your feet dry
- Use antifungal powders or sprays: Apply antifungal powders or sprays to your feet before putting on socks and shoes, especially if you are prone to fungal infections
- Avoid walking barefoot in public areas: Use protective footwear, such as flip-flops, when walking in communal showers, locker rooms, and pool areas
- Practice good foot hygiene: Wash your feet daily with warm, soapy water, and make sure to dry them thoroughly, paying attention to the areas between your toes
- Avoid sharing personal items: Do not share towels, socks, or shoes with others, as this can increase the risk of spreading fungal infections
By following these preventive measures, you can significantly reduce the likelihood of developing athlete’s foot.
Conclusion
Athlete’s foot is a common fungal infection that can cause discomfort and inconvenience. However, with proper treatment and preventive measures, it can be effectively managed and prevented. If you suspect you have athlete’s foot, it is essential to take prompt action to alleviate symptoms, prevent the spread of infection, and reduce the risk of complications. Ask your healthcare provider how you can keep athlete’s foot from spreading to other parts of your body or other people. If your symptoms persist or worsen despite self-treatment or if you have underlying health conditions speak to a healthcare professional. By practising good foot hygiene and implementing preventive strategies, you can keep your feet healthy and prevent the recurrence of athlete’s foot infections.
Sources
- Athlete’s foot – Symptoms and causes – Mayo Clinic
- What Is Athlete’s Foot & How Do You Treat It?
- Athlete’s foot – NHS
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.