Rheumatoid Arthritis Symptoms and Treatment

Rheumatoid arthritis (RA) is a chronic inflammatory systemic autoimmune disease that affects more than 400,000 people in the UK commonly between the age of 40 and 60 years. It is an autoimmune disease, meaning it occurs when your body’s immune system attacks its own tissues. While there is no known cure for rheumatoid arthritis, there are treatments available to help manage symptoms and reduce pain. Let’s take a look at what rheumatoid arthritis symptoms are, how they are diagnosed, and what treatment options exist.
What is rheumatoid arthritis?
Rheumatoid arthritis is an autoimmune and inflammatory disease that affects the lining of your joints, called the synovium. If you have rheumatoid arthritis, your immune system releases antibodies that attack the lining of your synovium, causing pain and inflammation. This inflammation can lead to scarring and joint damage over time, as well as pain and swelling. Rheumatoid arthritis is often grouped among other rheumatic diseases, along with conditions such as lupus, gout, and fibromyalgia. If left untreated, passive stiffness can become severe and cause total ankylosis (commonly referred to as frozen joint). Early diagnosis and treatment are always recommended to help reduce symptom severity and risk of further long term damage.
What are the three symptoms of rheumatoid arthritis?
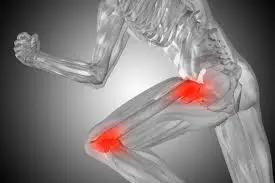
The symptoms of RA can cause problems in any joint in the body, although the small joints in the hands and feet are often the first to be affected. Both sides of the body are usually affected at the same time, in the same way, but this doesn’t always happen. The symptoms of RA can be divided into three main categories: joint pain, joint stiffness and swelling, and warmth and redness.
Joint pain
Pain is one of the most common symptoms of rheumatoid arthritis impacting up to 75% of RA patients, and can take many forms. For some people, the pain may be mild and occasionally present. Others may experience frequent and more severe levels of discomfort that can interfere with daily activities. Some have described flu-like intensity and stiffness when symptoms are at their peak. Pain in rheumatoid arthritis typically affects joints, as well as tendons, ligaments, and even muscles in extreme cases. It often occurs in flare-ups or episodes that can last for days or even weeks before subsiding again. Common areas for arthritic pain include the hands, feet, knees, shoulders and neck but can affect any part of the body.
Joint stiffness
Stiffness is a common and sometimes debilitating symptom of rheumatoid arthritis that can have a significant impact on mobility and quality of life. It occurs when the soft tissue found in and around the joint becomes inflamed, causing the muscles and surrounding ligaments to tighten. This can cause pain similar to holding your body in an uncomfortable position for long periods of time. People suffering from rheumatoid arthritis may experience this symptom especially first thing in the morning or after periods of rest or non-activity. In some cases, even the simplest of movements, such as bending at the waist or extending your arm outward, become difficult due to reduced joint range of motion and limitation of movement caused by stiffness. If left untreated, it can start to interfere with everyday activities like dressing and basic hygiene.
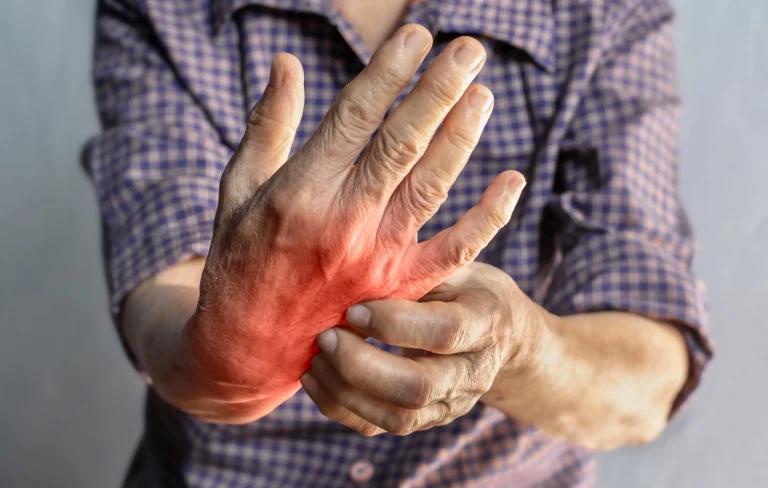
Swelling, warmth and redness
Rheumatoid arthritis (RA) can present with symptoms such as swelling of related joints, increased warmth to the touch in specified areas and redness. The swelling, warmth and redness are indicators of active inflammation and it is important to keep an eye out for these. These symptoms can be accompanied by rheumatoid nodules, which can appear firm and rubbery beneath the skin. They can appear on the skin as bumps and vary in size from about the size of a pea to the size of a golf ball. While difficult to observe in the hands, rheumatoid nodules are more easily identified in the elbows or other areas such as the feet and ankles.
Other symptoms
- Persistent fatigue and tiredness
- Unexplained weight loss
- Red eyes or dry eyes
Diagnosing Rheumatoid Arthritis
If you think you might be experiencing any of the above-mentioned symptoms, it’s important to make an appointment with your doctor right away. Before requesting certain tests your doctor will perform a physical exam and ask about your family history and other risk factors that put you at an increased risk of developing RA.
Blood tests
Diagnosing rheumatoid arthritis can be tricky; however, blood tests can help provide insight. C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) are two common tests that healthcare practitioners usually begin with.
CRP measures the level of an enzyme that gets released by your liver in response to inflammation. ESR checks for proteins in your blood that increase when there is an inflammatory reaction. Your doctor may also order a full blood count to check how many red and white blood cells you have. A full blood count looks for signs of infection and anaemia, both of which are common symptoms among sufferers. Knowing the results of these tests can give your healthcare provider a clearer picture of what treatment will best suit you.
Rheumatoid factor and anti-CCP antibodies
It can often be difficult to diagnose, so doctors may order a rheumatoid factor (RF) test and an anti-cyclic citrullinated peptide (anti-CCP) test, which may help to confirm a diagnosis of RA. These tests measure the chances of a person having RA by checking for specific markers in the blood that are linked to the disorder. While it is important to note that neither test alone conclusively proves if someone has RA, together they can provide valuable information that your doctor can use to determine whether you have the condition or not.
Scans
Joint scans are a common tool used by doctors to help diagnose rheumatoid arthritis. X-ray technology is utilised to identify areas of inflammation and joint damage in the body. With the help of x-rays, your doctor can assess how much joint damage has already occurred and may order additional scans over time to determine whether the disease is progressing or not. By looking at x-ray images from different angles, medical professionals can gain a better understanding of what is happening inside the joint and if it is indeed rheumatoid arthritis. The x-rays can also provide your doctor with the vital information they need to develop an effective treatment strategy.
Once all these tests have been completed, your doctor can diagnose whether or not you have rheumatoid arthritis and can refer you to a rheumatologist.
Treatment of Rheumatoid Arthritis
Once you have been diagnosed with rheumatoid arthritis, there are several treatment options available to help manage your symptoms and reduce pain levels.
Disease-modifying antirheumatic drugs (DMARDs)
Disease-modifying anti-rheumatic drugs (DMARDs). DMARDs help treat the underlying cause of your arthritis and deal with inflammation, joint destruction, and eventual disability caused by disease progression. They provide long-term relief of symptoms, reduce pain, and may slow down or stop further damage to joints. However, finding the right medication can take some trial and error as it works differently for everyone.
There are many different DMARDs that can be used, including:
- Methotrexate
- Leflunomide
- Hydroxychloroquine
- Sulfasalazine
- Other newer DMARDs, such as tofacitinib
While taking DMARDs can be beneficial in helping combat the pain and swelling of rheumatoid arthritis, some side effects may occur. These can include bruising and infectious risks such as flu-like symptoms; gastrointestinal issues like diarrhoea and nausea; and liver or kidney problems. Additionally, some drugs in this family could have an effect on other organs like your heart, lung and blood cells depending on what medicine you take.
Biological drugs
Biological treatments are one of the newer treatment options available for managing RA symptoms. Biological treatments are drugs derived from living sources, such as humans, animals or microorganisms. These treatments work by targeting specific molecules in the body that are part of immune system responses which contribute to inflammation in RA. The effects of these medications may be seen within days to weeks and, unlike traditional drugs, they work on an individual basis depending on what the patient needs; however, as with any serious medication, it is important to talk to your doctor about potential risks and possible side effects.
Pain relief
Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and COX-2 inhibitors are often prescribed to help manage the pain and swelling associated with rheumatoid arthritis. . Ibuprofen is a non-prescription medication that is widely available over the counter and long term use has been linked to gastrointestinal side effects such as ulcers and bleeding. For this reason, ibuprofen is usually the preferred option for short-term symptom relief. For prolonged treatment, your healthcare provider may recommend prescription COX-2 inhibitors such as celecoxib or etoricoxib which have less of an effect on the gastrointestinal tract. However, all NSAIDs carry their own risks so make sure to talk to your doctor before starting any new medication.
Steroids
Many people may be prescribed corticosteroids, also known as steroids, to help manage their arthritis symptoms. Steroids are potent medications which reduce inflammation, as well as controlling cell growth to decrease joint damage. Some examples of corticosteroids include prednisone and cortisone, which can be administered orally or by injection. Although corticosteroids can help manage pain, they are meant for short-term use due to potential side effects such as skin problems, weight gain and elevated blood glucose levels. Talk to your doctor or pharmacist if you are looking for more information about corticosteroids and how they could help with managing your rheumatoid arthritis symptoms.
Supportive treatments
For those suffering from rheumatoid Arthritis, there are several supportive treatments available to help manage their condition. Occupational therapists can provide exercises, lifestyle advice and tools to enable activities of daily living, as well as provide education about the condition. Physiotherapy can provide exercises to help maintain joint range of motion and reduce pain, while a podiatrist can treat orthopaedic problems and may also be able to help by providing aids such as splints or insoles. Other treatments may include occupational therapy strategies such as joint protection or pacing, relaxation techniques, assistive devices and/or other types of medication or therapies. Ultimately, the goal of supportive treatments is to aid in easing symptoms and enhancing the quality of life.
Surgery
Surgery for rheumatoid Arthritis can be a viable option for many patients seeking relief from pain and mobility issues. There are several types of surgeries available, including joint replacement, which repairs the damage caused by rheumatoid arthritis and improves flexibility and range of motion. Finger, hand and wrist surgery is a common choice that can help alleviate problems associated with carpal tunnel syndrome. This kind of procedure involves cutting away tissue to remove pressure on the median nerve in the forearm. Surgery can also help repair deformed joints, thereby restoring function and relieving soreness as well. Ultimately, it all comes down to what works best for you. Your doctor or surgeon will discuss your options with you in detail before making any decisions.
Dietary and lifestyle changes
Maintaining a healthy lifestyle can have a huge impact when it comes to managing rheumatoid arthritis. There have been many studies that demonstrate the importance of dietary and lifestyle modifications in helping to reduce common symptoms associated with joint pain and inflammation.
Taking supplements such as omega-3 fatty acid supplements, curcumin supplements, and magnesium supplements can all help enhance your RA treatment plan by improving levels of pain and reducing stiffness. In addition to supplements, incorporating foods like antioxidant-rich fruits and vegetables into your diet can help suppress inflammatory cytokines while improving overall health.
Regular exercise is also incredibly beneficial for anyone experiencing the effects of RA as staying active can improve physical function and help improve mobility and strengthen muscles around affected joints. Though dietary and lifestyle changes won’t automatically cure rheumatoid arthritis, taking small steps to incorporate healthier habits can make all the difference in day-to-day symptom management.
What is the difference between rheumatoid arthritis and osteoarthritis?
Rheumatoid arthritis and osteoarthritis are two types of arthritis, however, they have a few important differences. As mentioned earlier rheumatoid arthritis is an autoimmune condition in which the body’s own immune system attacks its own joint tissues causing inflammation that can damage cartilage and neighbouring bone. Osteoarthritis on the other hand is a degenerative disease primarily caused by mechanical stress on joints due to wear and tear from everyday use. Morning stiffness associated with osteoarthritis usually wears off within 30 minutes of getting up, but rheumatoid arthritis morning stiffness often lasts longer than this. Both rheumatoid arthritis and osteoarthritis can be managed through lifestyle modifications such as exercise, diet changes and receiving supportive care.
If you think you might be experiencing any of the common RA symptoms mentioned above or if you just want to learn more about the condition make sure to speak with your doctor, pharmacist or other healthcare professionals for medical advice. Early treatment and the right combination of medication and lifestyle changes means living with rheumatoid arthritis doesn’t have to mean living without a quality of life!
Sources
- Rheumatoid Arthritis – NHS
- Rheumatoid Arthritis (RA) – NRAS
- Rheumatoid Arthritis: A Brief Overview of the Treatment – NIH
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.