How Do You Tell if You Have a Blood Clot?

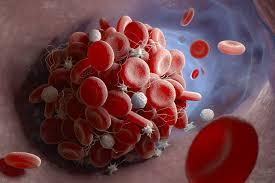
Blood clots are a common and potentially life-threatening medical condition that can occur in various parts of your body. Blood clots form when blood thickens and sticks together with platelets, proteins and other cells. While blood clots play a crucial role in the body’s natural healing process, they can become problematic when they block essential blood vessels, depriving tissues and organs of vital oxygen and nutrients.
Recognizing the early warning signs and symptoms of a blood clot is crucial, as prompt diagnosis and treatment can significantly improve outcomes and prevent serious complications. In this blog, we will explore the symptoms, causes, risk factors, and diagnostic procedures associated with blood clots, to help you safeguard your health.
Understanding blood clots
Blood clots, medically referred to as venous thromboembolism (VTE), can occur in various forms, each with its own set of symptoms and potential consequences. The two most common types of blood clots are deep vein thrombosis (DVT) and pulmonary embolism (PE).
Deep vein thrombosis (DVT)
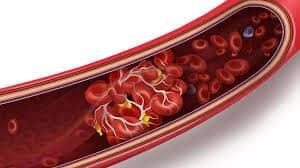
Deep vein thrombosis occurs when a blood clot forms in a deep vein, typically in the lower leg or thigh. These clots can cause pain, swelling, and discoloration in the affected limb. If left untreated, a DVT can break free and travel to the lungs, leading to a potentially life-threatening condition known as a pulmonary embolism.
Pulmonary embolism (PE)
A pulmonary embolism occurs when a blood clot, often originating from a deep vein, becomes lodged in the lungs, blocking blood flow and your oxygen supply. This can result in a sudden shortness of breath, chest pain, a rapid heartbeat, and in severe cases, loss of consciousness or even death.
Recognizing the symptoms
Identifying the symptoms of blood clots is crucial, as they can vary depending on the location and severity of the clot. It’s important to be aware of the following warning signs:
Symptoms of deep vein thrombosis (DVT)
- Swelling, typically in one leg or arm
- Pain or tenderness in the affected limb
- Redness or discoloration of the skin
- Feeling of warmth in the affected area
Symptoms of pulmonary embolism (PE)
- Sudden shortness of breath
- Chest pain, often worsening with deep breathing or coughing
- Rapid or irregular heartbeat
- Lightheadedness or fainting
- Coughing up blood
It’s important to note that some individuals may not experience any noticeable symptoms, making it even more crucial to be aware of the risk factors and to seek medical attention if any concerns arise.
Risk factors for blood clots
Certain factors can increase an individual’s risk of developing blood clots. Understanding these risk factors can help you and your healthcare provider take proactive steps to prevent and manage the condition. Key risk factors include:
Age
The risk of developing blood clots increases with age, particularly for individuals over the age of 60.
Immobility
Not moving for long periods of time, such as during extended hospital stays, long flights, or bed rest, can contribute to the development of blood clots.
Surgery and Injury
Damage to the blood vessel lining, often caused by surgical procedures or physical trauma can trigger the formation of blood clots.
Pregnancy and postpartum period
Pregnant individuals and those who have recently given birth are at a higher risk of developing blood clots due to the increased pressure in their veins and changes to the body’s clotting mechanisms.
Certain medical conditions
Conditions such as cancer, heart disease, obesity, high cholesterol, high blood pressure, inflammatory bowel disease, and certain inherited blood disorders can increase the risk of blood clots. A family history of blood clots can also increase your risk of blood clots.
Medications
Some medications, including birth control pills (oral contraceptives), hormone replacement therapy, and certain cancer treatments, can also contribute to an increased risk of blood clot formation.
Diagnosing blood clots
If you or your healthcare provider suspect the presence of a blood clot, a series of diagnostic tests may be ordered to confirm the diagnosis and determine the appropriate course of treatment.
Physical examination
Your healthcare provider will begin by conducting a thorough physical examination, assessing the affected area for signs of swelling, redness, and tenderness.
Imaging tests
- Ultrasound: This non-invasive imaging technique uses sound waves to visualize the blood flow in the affected veins, allowing for the detection of deep vein thrombosis
- CT Scan or an MRI: These advanced imaging tests may be used to identify blood clots in the lungs or other parts of the body
Blood tests
- D-dimer Test: This blood test measures the presence of a substance released when a blood clot breaks down to indicate the presence of a clot
- Coagulation Tests: These tests evaluate the body’s ability to form and dissolve blood clots, helping to identify any underlying clotting disorders
It’s important to note that a combination of these diagnostic tools may be used to confirm the presence and location of a blood clot, as well as to rule out other potential causes of the symptoms.
Treating blood clots
Once a blood clot has been diagnosed, your healthcare provider will work with you to develop a personalized treatment plan. The primary goals of treatment are to prevent the clot from growing larger, stop it from breaking free and traveling to other parts of the body, and to reduce the risk of future clots.
Anticoagulant medications
Blood thinners or anticoagulants are the mainstay of treatment for blood clots. These medications, such as heparin, warfarin, or newer oral anticoagulants, help prevent the formation of new clots and stop existing clots from growing larger.
Clot-dissolving medications
In some cases, healthcare providers may prescribe medications that help dissolve existing blood clots, particularly in more severe or life-threatening situations, such as a pulmonary embolism.
Compression stockings
Wearing compression stockings can help improve blood flow and reduce the risk of deep vein thrombosis, particularly in individuals who are at a higher risk or are recovering from surgery.
Surgical interventions
In rare cases, surgical procedures may be necessary to remove or break up a blood clot that is not responding to medication, or if the blood clot poses an immediate threat to the patient’s health.
It’s crucial to follow your healthcare provider’s instructions closely, take any prescribed medications as directed, and attend all scheduled follow-up appointments to ensure the successful management of your blood clot to prevent the development of future clots.
Preventing blood clots
While the risk of blood clots cannot be eliminated, there are several steps you can take to reduce your chances of developing this potentially serious condition:
Stay active and hydrated
Engaging in regular physical activity and staying well-hydrated can help improve blood flow and reduce the risk of clot formation, especially during extended periods of inactivity or travel.
Consider preventive medications
In some cases, your healthcare provider may recommend taking blood-thinning medications, such as low-dose aspirin or anticoagulants, to help prevent the formation of blood clots.
Use compression stockings
Wearing compression stockings, particularly during long flights or after surgery, can help improve blood flow and reduce the risk of deep vein thrombosis.
Quit smoking
Smoking is a significant risk factor for blood clots, so quitting or avoiding the habit can greatly reduce your chances of developing this condition.
When to seek medical attention
If you experience any symptoms that could indicate the presence of a blood clot, it is crucial to seek medical attention immediately. Prompt diagnosis and treatment are essential to prevent serious complications and potential life-threatening outcomes.
Call your healthcare provider or seek emergency medical care if you experience:
- Sudden, unexplained swelling, pain, or discoloration in a limb
- Sudden shortness of breath, chest pain, or a rapid heartbeat
- Coughing up blood
- Lightheadedness or fainting
Early recognition and intervention can make all the difference in the successful management of blood clots, so don’t hesitate to seek medical if you notice any signs or symptoms. If you have any pre-existing medical conditions that increase your risk of blood clots, it is likely that your healthcare provider will be advising you on managing those risks.
Conclusion
Blood clots are a serious medical condition that can have potentially life-threatening consequences if left untreated. By understanding the symptoms, risk factors, and diagnostic procedures associated with blood clots, you can take proactive steps to protecting your health.
It is essential to be vigilant about any changes in your body and to work closely with your healthcare provider to develop a comprehensive plan for the prevention, early detection, and effective management of blood clots, especially if you have higher risks.
Sources
- Blood clots – NHS
- Blood clots risk – CDC
- Deep Vein Thrombosis – Mayo Clinic
- The basics of blood clots what you need to know – Medline Plus
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.