Everything You Need to Know About Monkeypox

The first case of Monkeypox in the U.K was confirmed by the World Health Organisation (WHO) in May 2022. The case involved a person who made a journey from the United Kingdom to Nigeria and later returned to the United Kingdom. The number of confirmed cases of monkeypox in the United Kingdom is 524, as of 14 June. This can be broken down by each country: 504 confirmed cases in England, 13 in Scotland, 2 in Northern Ireland and 5 in Wales. These results are from the UK Health Security Agency (UKHSA).
The World Health Organisation is currently in talks to firstly determine if the current outbreak of monkeypox is a public health emergency and secondly they are working with experts to come up with a new name for monkeypox. The name change has been urged by over 30 leading scientists who want a neutral, non-discriminatory and non-stigmatising replacement name.
Health officials predict that monkeypox will not produce a pandemic situation comparable to the coronavirus. Read on to find out what monkey pox is, its symptoms and how it is transmitted.
What is monkeypox?
Monkeypox was first discovered in the 1970’s and is not a new disease as commonly thought, with the Democratic Republic of the Congo recording the first human case. Monkeypox has been endemic in West Africa and Central Africa for decades, but we have now seen non-endemic countries experiencing monkeypox outbreaks including Europe.
It is a rare infectious disease that is caused by the monkeypox virus which is closely related to the small pox virus but not related to chickenpox. Monkeypox virus is part of the Orthopoxvirus genus in the family Poxviridae. This genus also includes variola virus (which causes smallpox), vaccinia virus (used in the smallpox vaccine), and cowpox virus.
In 1958 the first outbreak of monkeypox occurred in colonies of monkeys kept for research and this is how the disease gained its name however the source of the disease is still undiscovered. It is known however, that African rodents and non-human primates (like monkeys) may conceal the virus and infect people.
What is the treatment for monkeypox?
The genetically similar nature of monkeypox and smallpox means that the medications developed for smallpox can be used to treat monkeypox. The type of drugs used are anti-viral drugs and vaccines. Your clinician can give you more information on the type of drugs available.
20,000 plus doses of the smallpox vaccine Imvanex have been acquired by UKHSA to treat close contact associates of those diagnosed with monkeypox to reduce the risk of symptomatic infection and severe illness. The United Kingdom is already offering vaccines to health care workers and other contacts of known cases. This strategy is called ring vaccination, which was used to wipe out smallpox effectively.
What are the symptoms of monkeypox?
There are two clades of the monkeypox virus: the West African clade and the Congo Basin (Central African) clade. Human infections with the West African clade appear to cause less severe symptoms.
According to the CDC (Centers for Disease Control and Prevention) it can take between 7-14 days or 5-21 days from infection to symptoms for monkeypox to appear.
The first symptoms normally seen are:
- High temperature
- Swollen lymph nodes (lymphadenopathy)
- Headache
- Muscle aches
- Backache
- Exhaustion
- Chills
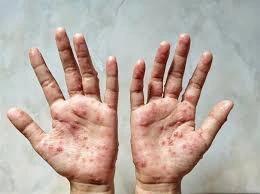
1-5 days after the first symptoms a rash on the face and other parts of the body, including the genital area starts to develop.
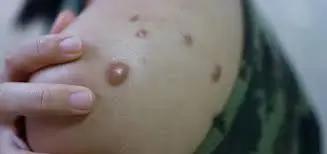
Skin lesions progress through the following stages before eventually falling off:
- Macules (skin colour change)
- Papules (raised bump)
- Vesicles (fluid filled sac)
- Pustules (blister containing pus)
- Scabs (dry rough crust)
Monkeypox typically lasts for 2−4 weeks. Monkeypox is usually mild and most people recover without treatment.
What should I do if I have symptoms?
- Make contact with your healthcare provider if you observe a new or unexplained rash or other monkeypox symptoms shown above
- Remind the healthcare provider that monkeypox is circulating
- Until a healthcare professional examines you do not engage in any form of close contact (including intimate physical contact) with others
- No close contact with pets or other animals until you see a doctor
- All the above safety measures should be followed if you’re waiting for test results
- You must isolate if your test is positive and remain isolated until all scabs have fallen off and new fresh skin has appeared
How do I get monkeypox?
Monkeypox can spread in three different ways:
- Contact with an infected animal that has bitten you or contact with its blood, body fluids, spots, blisters or scabs
- Human transmission involves contact with an infected person such as close contact, touching parts of the body with monkeypox lesions, and direct contact with body fluids, or respiratory droplets including sexual contact, kissing and cuddling
- Contact with materials contaminated with the virus such as bedding or clothing
Key differences between monkeypox and smallpox
- Symptoms of monkeypox are milder than smallpox
- Smallpox spreads more easily than monkeypox
- Monkeypox causes lymph nodes to swell while smallpox does not
Tips to avoid getting monkeypox while travelling
- Adhere to basic hand-washing rules. Ensure you wash your hands with soap and water frequently. Keep an alcohol-based hand sanitiser in your bag
- Eat food that has been well-cooked, particularly meat
- Stay away from wild or stray animals, including dead animals
- Keep your distance from any animals that appear unwell
- Do not eat or touch meat from wild animals (bush meat)
- No sharing of bedding or towels with people who are unwell and may have monkeypox
- No close contact with people who are unwell and may have monkeypox
Sources
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.