What Is Raynaud’s Disease?

(Current Version)
If you’re here, then you may have noticed unexplained changes in the colour of your skin, especially your fingers and toes. The discomfort from this is likely due to Raynaud’s disease, a condition that affects both men and women of any age. Not everyone who experiences discolouration has Raynaud’s Disease, but it can be an indicator as there are several known triggers for the disorder. In this blog post, we’ll dive into more detail about what exactly Raynaud’s Disease is and what ways there are to manage its symptoms.
What is Raynaud’s disease?
Raynaud’s disease, also known as Raynaud or Raynaud’s Phenomenon, is a condition that causes certain areas of the body to experience reduced blood flow. Mainly the fingers, toes, nose and ears when exposed to cold temperatures or extreme stress. It is more common among women than men and often affects those younger than 30 years of age.
What causes Raynaud’s syndrome
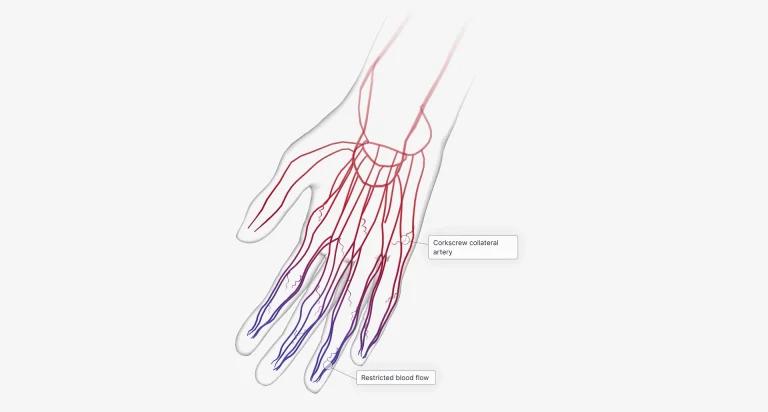
Raynaud’s syndrome is a condition caused by an abnormal response in the body’s blood vessels. It occurs when the small arteries that supply blood to your skin narrow and reduce the flow of blood to your fingers, toes, nose and ears. In some cases, these arteries can become so narrow that they nearly close off completely. When this happens, it causes pale or bluish skin discolouration and numbness or tingling on the affected parts of the body.
This could be due to genetics, autoimmune diseases, vascular disease or even certain medications. However, among those who are affected, it is frequently discovered that no specific causes of Raynaud can be identified. Instead, specific triggers or risk factors are commonly found to induce Raynaud’s attacks. This may include living in extreme temperatures (cold or hot), emotional stress, a family history of the disease or even something as simple as typing or reaching into a refrigerator.
Medication side effects and drug interactions can cause an exacerbation of Raynaud’s Disease. Beta-blockers and ergot derivatives are two types of common medications that can aggravate Raynaud’s Disease symptoms. Beta-blockers are used to treat high blood pressure, heart and chest pain, migraines and other cardiovascular diseases. While ergot derivatives such as vasoconstrictors, triptans, lithium, dopamine agonists and antipsychotics are often prescribed to treat mental health conditions.
Other medications that may cause this phenomenon include diuretics/water pills (used to aid in water management within the body), oestrogens (hormone therapy used for contraception or menopausal symptoms), selective serotonin reuptake inhibitors (anti-depressants), taxanes (drugs used to treat specified cancers) and some forms of chemotherapy agents. It is important to ask your doctor about the potential risks associated with these medications before taking them.
Different types of Raynauds
There are two types: Primary Raynaud’s phenomenon and Secondary Raynaud’s phenomenon.
Primary Raynauds
The majority (80–90%) of individuals with Raynaud disease have primary Raynaud’s phenomenon. It has no known underlying cause but experts believe it could be a result of an overactive reflex when exposed to cold temperatures causing a narrowing of the arteries or veins due to vasospasms.
In some cases, genetics plays a role in increased sensitivity and reactions to external triggers. Other possible contributing factors include smoking, stress and medications that cause constriction of blood vessels leading to episodes of Raynaud’s symptoms. While no one knows what exactly causes Primary Raynauds, there are steps that can be taken to help diminish its symptoms and reduce the frequency of attacks.
Secondary Raynaud
Secondary Raynaud is a condition associated with other underlying conditions and can be caused by such things as working with vibrating tools, certain medications, atherosclerosis and systemic diseases. The most common form of Secondary Raynaud’s phenomenon is related to scleroderma and other autoimmune connective tissue diseases such as Sjogren’s Syndrome, Carpal Tunnel Syndrome, Scleroderma, Lupus or Rheumatoid Arthritis.
Symptoms of Raynauds
Raynauds Disease causes episodes of disrupted blood flow in the small blood vessels in the hands and feet due to extreme sensitivity to cold.
- It is characterised by colour changes in the affected area
- Tender or tingly sensation in the affected area and a gradual progression into numbness when exposed to colder temperatures
- During these episodes, the fingertips, toes and other extremities turn white as circulation stops oftentimes followed by a blue hue, then red once blood flow returns to the area
Severe Raynaud symptoms may include:
- Persistent joint pain
- Ulcerations on fingertips
- Gangrene which in rare cases may lead to finger or toe amputation
The frequency and duration of these events vary from person to person, but often begin with shorter-duration attacks that become more severe over time.
If you think you may have Raynaud disease because of constant or sudden changes in your skin discolouration, it is important to speak with your healthcare provider for further guidance on how best to manage your symptoms.
Diagnosis of Raynaud’s disease
Diagnosis for Primary Raynaud’s can be achieved through a physical exam and patient history. Your doctor will examine your skin and your nails for colour changes and look for signs of tissue damage during a Primary Raynaud diagnosis. During a primary Raynaud test, doctors will also check for sensitivity to cold temperatures or vibration by performing tests such as the nail fold capillaroscopy or the finger-temperature test.
Similarly, Secondary Raynaud’s is diagnosed with an assessment of medical history along with medical examinations such as Thermal Quantitative Sweat Testing, to look at the performance of sweat glands based on temperature, and X-Ray imaging to look for additional evidence of any connective tissue ailments associated with Primary Raynaud’s.
To rule out secondary Raynaud’s, blood tests might also be necessary to eliminate other possible causes for similar symptoms.
An Erythrocyte sedimentation rate (ESR) test is a simple lab test used to determine inflammation in your body. This test measures the rate of red blood cells that fall toward the bottom of a sample tube. Normally, an increased sedimentation rate could indicate that there is an underlying inflammatory or autoimmune disease, such as rheumatoid arthritis and other medical conditions. An ESR test is a non-invasive procedure that will only involve a small sample of your blood being taken from a vein in your arm. Blood tests measure levels of substances called antibodies, which can indicate an underlying autoimmune condition associated with SRS.
Treatment of Raynaud Disease
Although there is no cure for Raynaud’s disease, various treatments are available to help manage symptoms and improve the overall quality of life. Treatment plans vary from patient to patient but usually involve lifestyle modifications and medication.
Lifestyle
Additionally, lifestyle modifications such as quitting smoking, avoiding stimulants (coffee and soda), eating a balanced diet rich in Omega-3 fatty acids and increasing exercise and strength training, can help reduce its severity.
Medication
Your doctor may prescribe medications including vasodilators, calcium channel blockers, antidepressants and biologics for more severe cases of Raynaud’s disease.
Nifedipine
Nifedipine is an oral medication that is commonly used to treat this condition. As a calcium channel blocker, nifedipine helps relax arteries and improves circulation by increasing blood flow throughout the body. It may also help reduce symptoms such as pain and numbness associated with Raynaud’s Disease.
This is the only medicine licensed to treat Raynaud’s phenomenon in the UK. Although it should be noted that nifedipine does not provide a cure for Raynaud’s Disease, it can greatly improve the quality of life for those suffering from this condition.
It is important that you follow your doctor’s instructions carefully in order to minimise potential risks associated with treatment as well as to see maximum benefit from your prescribed treatments.
Other medications
Sildenafil, also known as Viagra has some evidence of benefits for Raynauds symptoms. Sildenafil works by preventing the constriction of these blood vessels, allowing blood to restore normal flow to the affected area. Clinical trials have shown promising results, with some patients reporting improved blood flow and decreased pain after just one dose. While side effects can occur, they are mild and typically subside quickly.
Another potential way to manage Raynaud’s disease is through medication such as antidepressants. The antidepressants work by altering the body’s response to changing temperatures, thereby reducing symptoms associated with the condition. Different types of antidepressants may be prescribed and it should be noted that this type of treatment is not suitable for everyone. Your doctor will assess your individual situation and discuss with you if this approach is likely to provide benefits in managing your condition.
Healthcare professionals may prescribe Sildenafil or an antidepressant as part of a comprehensive treatment plan tailored to each individual’s unique needs. These medicines are not licensed for the treatment of Raynaud’s in the UK, but you may be prescribed them if it’s thought the potential benefit outweighs the possible risks. Rheumatology can provide other options for treatment depending on a patient’s unique medical history and presentation of symptoms.
Practical tips for people with Raynaud Disease
Living with Raynaud’s Disease can be challenging, yet following some practical tips can make all the difference in helping to manage and control the symptoms
- Keep your hands and feet warm by wearing several layers of clothing and accessories like hats, scarves, gloves and leg warmers when going outside during cold weather months
- Investing in warm thermal socks is also a great way to help stabilise body temperature
- Avoiding extreme temperatures or sudden changes in temperature will help prevent an attack. Even relatively minor exposure to the cold, such as holding a glass of ice-cold water or being in air conditioning, can cause the change
- Keeping stress levels low is essential as stress has been shown to trigger
- Learning relaxation techniques such as yoga can also be beneficial
- Eating certain foods can also help improve circulation and reduce inflammation. Foods high in omega-3 fatty acids such as salmon, mackerel and sardines, as well as antioxidants like strawberries, blueberries, tomatoes and red bell peppers are recommended for their anti-inflammatory properties
- Avoid repetitive actions, such as typing or use of tools that vibrate like a jackhammer
Seek help and support
Raynaud’s disease can have a serious impact on your quality of life if left untreated, so it’s important to speak with your healthcare provider if you think you might have this condition. With proper treatment and lifestyle modifications, many people are able to manage their symptoms effectively and live an active life despite having Raynaud’s disease. If you think you may have this disorder, don’t hesitate to talk to your doctor about diagnosis and treatment options that could help improve your quality of life.
SRUK is a charity for people with scleroderma and Raynaud’s. It offers further information and advice about living with Raynaud’s and information on how to find support groups.
Sources
- Raynauds – NHS
- Raynaud’s phenomenon – NCBI
- Scleroderma & Raynaud’s UK – SRUK
- Raynaud’s phenomenon – Niams
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.




