What Is the Cause of Autoimmune Diseases?

Autoimmune diseases affects millions worldwide. These disorders arise when the body’s immune system attacks its healthy cells and tissues. This self-destructive response targets various organs, glands, and bodily systems, leading to a range of symptoms and consequences.
Uncovering the root causes of autoimmune diseases has long been a challenge for the medical community. Experts have identified several key risk factors that likely contribute to the development of these different autoimmune diseases.
The role of the immune system
At the core of autoimmune diseases is a breakdown in the normal functioning of the immune system. The immune system, which is designed to protect the body from external threats such as pathogens, infections, and cancer cells, fails to distinguish between self and non-self in autoimmune disorders.
Normally, the immune system has a delicate balance between activating and suppressing its response to maintain a balanced body. In autoimmune diseases, this balance is disrupted, leading the immune system to mistakenly attack the body’s own healthy cells and tissues.
This immune response can be triggered by a variety of factors, including genetics, environmental exposures, and even hormonal imbalances. The specific mechanisms by which the immune system becomes unbalanced can vary depending on the type of autoimmune disease, but the result is the same: a cycle of inflammation, tissue damage, and disease progression.
The complexity of autoimmune diseases
Autoimmune diseases are remarkably diverse, with over 80 conditions recognised by the medical community. Some of the most well-known autoimmune disorders include:
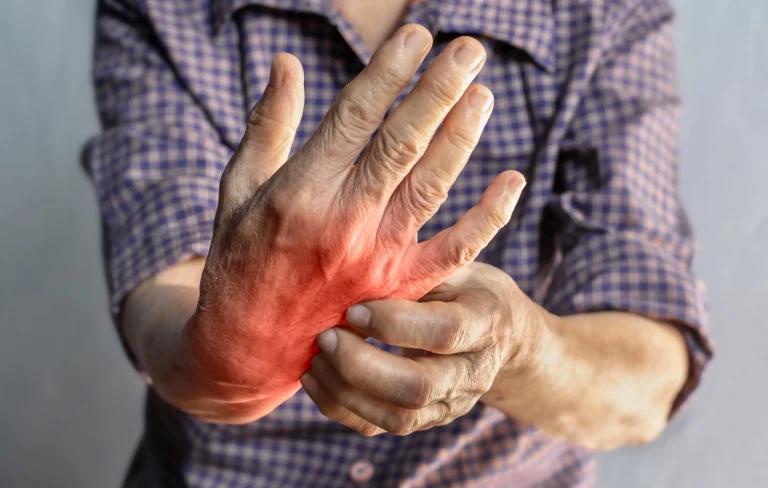
- Rheumatoid Arthritis: An inflammatory condition that targets the joints, causing pain, swelling, and stiffness
- Lupus: A chronic disorder that can affect various organs, including the skin, connective tissues, and kidneys
- Multiple Sclerosis: A neurological condition in which the immune system attacks the protective myelin sheath surrounding nerve fibres, disrupting communication within the central nervous system
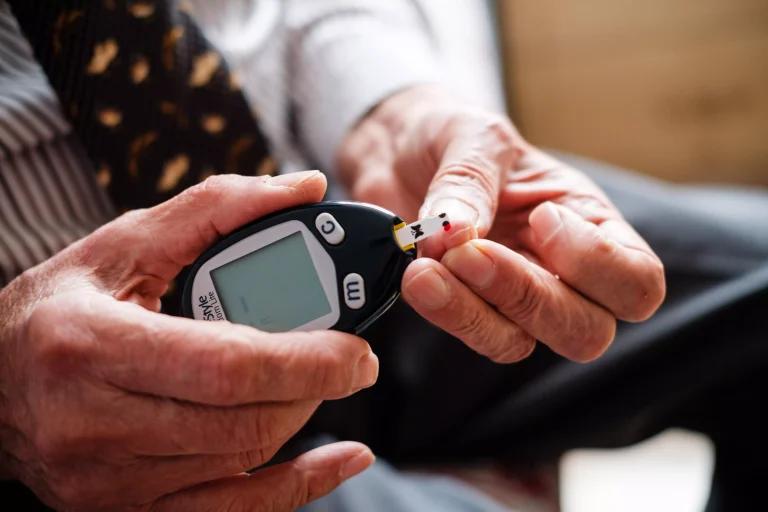
- Type 1 Diabetes: An autoimmune disease that destroys the insulin-producing cells in the pancreas, leading to an inability to regulate blood sugar levels
- Inflammatory Bowel Diseases (Crohn’s Disease and Ulcerative Colitis): Conditions characterised by chronic digestive tract inflammation
- Hashimoto’s Thyroiditis: An autoimmune disorder that targets the thyroid gland, leading to hypothyroidism and a range of hormonal imbalances
- Graves disease is an autoimmune disorder that involves overactivity of the thyroid hormone (hyperthyroidism)
- Psoriasis: An autoimmune skin condition that causes the rapid buildup of skin cells, resulting in scaly, red patches
Patients may experience a wide range of symptoms in all parts of the body, from joint pain and fatigue to skin rashes and digestive issues, making it difficult for healthcare providers to pinpoint the underlying cause.
Genetics
Numerous studies have revealed that certain genetic variations can put individuals at a higher risk of developing these disorders. Specific gene mutations or combinations of genes can alter the normal functioning of the immune system and mistakenly identify the body’s cells as foreign invaders.
This genetic component often runs in families, with individuals who have a close relative with an autoimmune disease being at a higher risk of developing a similar condition themselves. The inheritance patterns can be complex, with multiple genes typically involved in the disease process. Additionally, certain ethnic and racial groups may have a higher genetic susceptibility to particular autoimmune disorders.
Environmental triggers
Environmental influences can also significantly contribute to autoimmune diseases. Various environmental exposures, such as viral or bacterial infections, certain chemicals, and even physical and emotional stressors, can be triggers for the immune system’s response.
Furthermore, stress, both physical and psychological, has been linked to the development and worsening of autoimmune conditions. Chronic stress can impair the immune system’s ability to function properly, increasing the risk of autoimmune disorders.
Gender
Autoimmune conditions are far more common in women than in men, with estimates suggesting that up to 80% of those affected are female.
Researchers have proposed several reasons to explain this difference, including the potential role of hormonal factors, genetic differences, and even the influence of the X chromosome. Estrogen, for instance, has been found to play a complex role in the regulation of the immune system, and fluctuations in its levels may contribute to the increased susceptibility of women to autoimmune diseases.
Additionally, the X chromosome contains a significant number of genes involved in immune function, and the presence of two X chromosomes in women may result in a higher risk of autoimmune disorders compared to the single X chromosome in men.
The gut microbiome
In recent years, the gut microbiome has been highlighted as a key factor in the development and progression of autoimmune diseases. The gut microbiome, the diverse community of microorganisms that live within the human gastrointestinal tract, plays a crucial role in immune system function and the prevention of autoimmune responses.
Imbalances in the gut microbiome, often triggered by factors such as diet, antibiotic use, and environmental exposures, have been linked to various autoimmune conditions. These microbial imbalances can disrupt the delicate balance between the gut and the immune system, leading to increased inflammation and the development of autoimmune illnesses.
Sex hormones
Estrogen, the main female sex hormone, has been found to play a role in the regulation of the immune system. Changes in estrogen levels, such as those experienced during pregnancy, menstrual cycles, and menopause, can impact the delicate balance of the immune response, potentially contributing to autoimmune disorders.
Testosterone the main male sex hormone, on the other hand, has been associated with a more regulated and balanced immune response, potentially offering some protective effects against autoimmune diseases.
Age and ethnicity
The risk of developing autoimmune diseases can also be influenced by an individual’s age and ethnicity.
Certain autoimmune conditions, such as type 1 diabetes and juvenile rheumatoid arthritis, tend to occur more frequently in childhood and adolescence, while others, like rheumatoid arthritis, are more common in older adults. This age-related risk suggests that the maturation and changes in the immune system over the lifespan may play a role in the development of autoimmune disorders.
Some ethnic and racial groups have been found to have a higher prevalence of specific autoimmune diseases. For example, individuals of African, Asian, and Hispanic descent may be at an increased risk of developing lupus, while Caucasians are more susceptible to conditions like multiple sclerosis and rheumatoid arthritis. These differences likely reflect a mixture of genetic, environmental, and cultural factors.
Diagnosis
Healthcare providers often rely on a combination of medical history, physical examination, laboratory tests, and imaging studies to piece together the puzzle and arrive at a diagnosis.
Blood tests, such as the antinuclear antibody test (ANA test) can provide valuable clues, but the unpredictable nature of autoimmune diseases, with periods of remission and flare-ups, can also make it difficult to obtain a clear picture.
Early treatment
Prompt treatment of these conditions can help reduce the progression of tissue damage, prevent the development of complications, and improve the overall quality of life for patients. Delays in treatment can have significant consequences, as untreated autoimmune diseases can lead to irreversible organ damage, disability, and even life-threatening complications. Raising awareness among healthcare providers and the general public about the early signs and symptoms of autoimmune diseases is important.
Conclusion
Significant progress has been made in understanding the underlying causes of autoimmune conditions but continued research remains to be done. Genetics, environmental triggers, gender, age, ethnicity, and the gut microbiome all contribute to the unpredictability of these disorders.
Sources
- Autoimmune Diseases: Types, Causes, Symptoms & Treatment
- Autoimmune Diseases – Autoimmune Disease Symptoms – MedlinePlus
- National Institute of Environmental Health Sciences: Autoimmune Diseases
- Autoimmune disorders: MedlinePlus Medical Encyclopedia
-
Medical Disclaimer
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.