What Is Chronic Insomnia?

Insomnia is a common sleep disorder that makes it difficult for people to fall asleep, stay asleep or fall asleep again if they wake up at the night. Insomnia affects your sleep quality and your mood, general health and overall quality of life. Insomnia is more prevalent in women than men.
Chronic Insomnia (also known as chronic insomnia disorder) is when the symptoms generally last for prolonged periods, at least three nights a week for a month or longer. In contrast, acute insomnia usually lasts a few days or around a week. It is also known as short-term insomnia. Primary insomnia is where your sleep problems aren’t linked to other health conditions or issues.
What are the symptoms of chronic insomnia?
Insomnia symptoms may include:
- Difficulty falling asleep at night
- Waking up during the night
- Feeling tired
- Daytime sleepiness
- Irritability, depression or anxiety
- Difficulty focusing, concentration impairment
- Stressing about sleep
If insomnia makes it hard for you to function during the day, see your doctor to identify the cause of your sleep problem and how it can be treated. If your doctor thinks you could have a sleep disorder, you might be referred to a sleep centre for special testing.
What causes chronic insomnia?
Common risk factors of chronic insomnia include:
- Stress about work, school, health, finances or family
- Disrupting your body’s circadian rhythms – causes include jet lag from travelling
- Poor sleep habits such as naps, an uncomfortable sleep environment, poor sleep hygiene, watching TV in bed, using smartphones or using other screens just before bed
- Overeating late in the evening
Other common causes of insomnia include:
- Mental health disorders such as anxiety disorders, post-traumatic stress and depression
- Medications such as antidepressants, treatments for asthma or blood pressure
- Over-the-counter medicines that contain caffeine and other stimulants
- Medical conditions – chronic pain, cancer, diabetes, heart disease, asthma, gastroesophageal reflux disease, overactive thyroid, Parkinson’s disease, degenerative neurological disorders and Alzheimer’s disease
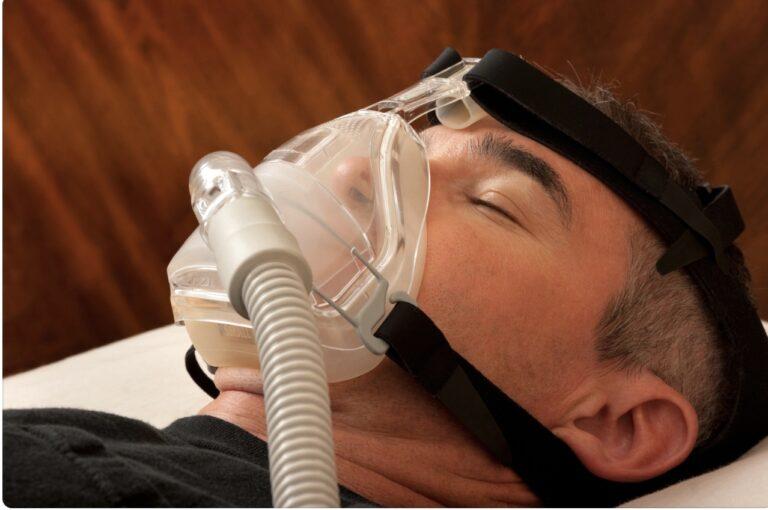
- Sleep apnea – can cause you to stop breathing periodically throughout the night, interrupting your sleep
- Restless legs syndrome may prevent you from falling asleep
- Having drinks that contain caffeine which is a stimulant before going to bed. The American Academy of Sleep Medicine recommends that you stop drinking caffeinated drinks at least six hours before bedtime
- Insomnia is more common in older adults due to changes in sleep patterns, how active they are, as well as changes in health and medication
- Being a woman – pregnancy, the menstrual cycle and menopause may play a role in changing sleep patterns
- Not having a regular sleep schedule, e.g. rotating shift work or travelling can cause sleep loss
A lack of sleep can cause huge health problems in terms of sufferers’ physical and mental well-being. Chronic insomnia puts your body under pressure and increases medical conditions such as diabetes, strokes, heart attacks, seizures and high blood pressure. It can also impact your sex drive, your memory and your judgment. Being low on energy can lead to feelings of anxiety, depression, or irritation.
Treatments for insomnia
Treatment of insomnia can range from behavioural therapy, prescriptions for sleeping pills from a doctor or over-the-counter sleep aids. Some contain natural ingredients (valerian, lavender or melatonin), while others, like Nytol, are antihistamines.
Before speaking to a healthcare professional, it is worth looking at your lifestyle and making changes to see how that impacts on your insomnia.
- Try changing your sleep habits, daily routine and attitude about sleep. Evidence shows that lifestyle and behavioural changes make the largest and most lasting difference when it comes to insomnia
- Exercise can be a great help, however, don’t exercise close to bedtime, or it could have a reverse effect
- Taking a bath an hour before bed and not using mobiles a few hours before you go to sleep can help make you feel relaxed
- Sleeping aids are available over the counter from your Pharmacist. These can help to relax the body, but they do have side effects, including drowsiness
Your doctor will do a physical exam and ask about your medical and sleep history. They might tell you to keep a sleep diary for a week or two, keeping track of your sleep patterns and how you feel during the day. They may talk to your bed partner about how much and how well you sleep. You might also have special tests at a sleep centre.
- Cognitive behavioural therapy for insomnia (CBT-I) is the recommended first-line treatment for chronic insomnia. Medications may be used as an adjunct to CBT-I, but their long-term effectiveness and safety have not been well assessed. CBT can help promote good solid sleep at night. Some techniques you may learn in behaviour therapy will include exercises that cause relaxation, reconditioning yourself and sleep restriction therapy. These techniques will help you relax, fall asleep and stay asleep longer
- One behavioural approach, called stimulus control therapy, aims to break harmful sleep habits and thoughts over the course of several weeks
- There are also dietary and herbal treatment options to help you get good sleep if you are having trouble sleeping. Although they may be described as “natural,” be aware that sleep remedies can still have side effects and interfere with other medications or vitamins you’re taking. For more information, talk to your doctor or pharmacist. The two supplements with the most evidence supporting their effectiveness for insomnia are melatonin and valerian. Melatonin is a naturally occurring hormone that your body produces at night. It helps regulate your sleep cycle but may not work for everyone. Valerian is a herb with mild sedative effects that may help you sleep better
- Sleeping pills (hypnotics) are usually the last resort but are not prescribed as widely by GPs as they used to be due to the addictive nature of the tablets. Prescription sleep medications can give temporary relief. It’s important to understand that sleeping pills are not a cure for insomnia. If not used carefully, they can worsen insomnia in the long run. It’s best to use medication as a last resort and only on a limited, as-needed basis
Sources
NowPatient has taken all reasonable steps to ensure that all material is factually accurate, complete, and current. However, the knowledge and experience of a qualified healthcare professional should always be sought after instead of using the information on this page. Before taking any drug, you should always speak to your doctor or another qualified healthcare provider.
The information provided here about medications is subject to change and is not meant to include all uses, precautions, warnings, directions, drug interactions, allergic reactions, or negative effects. The absence of warnings or other information for a particular medication does not imply that the medication or medication combination is appropriate for all patients or for all possible purposes.




